Vector Borne Diseases and COVID-19

What are vector borne diseases?
Vector-borne diseases are infections caused by parasites, viruses and bacteria and transmitted by vectors, which are usually the insects. They ingest pathogens while taking a blood meal from an infected host (human or animal) and transmit it into a new host, after the pathogen has multiplied inside them. Once a vector becomes infectious, it remains so for the rest of its life, transmitting the infection during each subsequent bite/blood meal.
Several insects serve as vectors for many diseases and mosquitoes are the most common type. Different genera of mosquitoes serve as vectors for different diseases. For example:-
- Aedes mosquito serves as vector for Dengue,Chikungunya, Yellow Fever and Zika
- Anopheles as vector for Malaria
- Culex as a vector for Japanese Encephalitis.
All the three species of mosquitoes can serve as vectors for Filariasis. Other insects including rat fleas act as vectors for plague (transmitted from rats to man), sandflies for Kala-azar, chiggers (larvae) of mites for Scrub Typhus; ticks and lice can also serve as vectors.
Rise of Vector Borne diseases in India
- Vector borne diseases have been a major health burden for the under-developed as well as the developing countries including India for many decades.
- According to the WHO report, one sixth of the illness and disabilities suffered worldwide are due to vector-borne diseases, with more than half the world’s population currently estimated to be at risk of these diseases.
- Inadequate containment of the vectors has resulted in recurrent outbreaks and re-emergence of the vector-borne diseases.
Spread of Vector Borne diseases
- Vector borne diseases occur by the bites of the infected vectors.
- An epidemic process relies heavily on the availability of suitable environmental and climatic conditions. The commencement of the monsoons marks the beginning of a sharp rise in the number of cases of these vector-borne diseases, as the climate becomes conducive for the breeding of vectors.
- Mosquitoes and other vectors usually breed in polluted water bodies, overhead tanks and stagnant water bodies.
Vector Borne diseases prevalent in india
The important vector borne diseases prevalent in India include Malaria, Dengue, Chikungunya, Filariasis, Japanese Encephalitis, Kala Azar and Scrub Typhus.
Malaria
- Malaria is caused by plasmodium parasites, transmitted through bites of infected anopheles mosquitoes.
- Populations who are at risk include young children, pregnant women, people living with HIV, those affected by humanitarian emergencies and natural disasters, and non-immune travellers moving into endemic areas.
- Five parasite species cause malaria in humans. Plasmodium falciparum and P. vivax are the most common, while P. falciparum is the most dangerous species with the highest rates of complications and mortality. Malaria mosquitoes usually bite at night.
- Symptoms of malaria include high grade fever, with chills and rigor, headache, body ache, and non-specific symptoms like nausea, vomiting, dry cough, etc.
- Malaria when left untreated may result in severe malaria, manifesting into certain danger signs requiring immediate attention. This includes jaundice, liver failure, bleeding from any site, unconsciousness, seizures, inability to pass urine, kidney failure, multi-organ failure and occasionally death.
- Certain patients experience symptoms including severe headache, seizures, internal/external bleeding, as well as development of jaundice.
- Early diagnosis can be made by a simple blood test, with results obtained in a few minutes.
- Treatment of malaria includes rest and fever control (with paracetamol), cold sponging and oral medications for a few days. Severe malaria requires intravenous drugs. Infants and pregnant women require special attention.

Dengue
- Dengue fever is caused by the dengue virus and gets transmitted by the Aedes mosquito.
- It is commonly known as the tiger mosquito, due to the stripes on its legs and wings.
- This mosquito usually bites early in the morning and before dusk in the evening.
- The Aedes breeds in freshwater pools and man-made containers.
- Dengue occurs as epidemic forms from time to time. Its common name is breakbone fever. All age groups and both sexes are vulnerable.
- The four known serotypes of dengue virus are DEN 1 to 4. Recovery of a patient from infection by any one of these viruses provides lifelong immunity against that particular serotype. However, these subsequent infections by other serotypes of this virus increase the risk of developing severe dengue. Thus, individuals who are previously infected by dengue are more likely to experience a severe form of the disease if re-infected.
- The cases of dengue usually peak from the months of July to December.
- Symptoms include high fever, rashes, severe headaches, muscle and joint pains, pain behind the eyes, nausea, or vomiting. Dengue itself is rarely fatal, but severe dengue is a potentially fatal complication, with symptoms including low temperature, severe abdominal pains, rapid breathing, and bleeding.
- Decrease in platelet count leads to bleeding from several sites including gums, into the joints, under the skin. This leads to discolouration, and even black coloured stools or frank blood in stools.
- Danger signs requiring immediate attention include bleeding from any site, severe abdominal pain, prolonged frequent vomiting, unconsciousness, and high grade fever.
- The treatment includes adequate fluids and rest, along with Paracetamol for pain and fever, and continuous monitoring of platelet count and blood pressure. There are no effective antiviral medications to treat dengue infection. In cases of severe dengue, it is critical to maintain the patient’s body fluid volume and if required undergo platelet transfusion or blood transfusion.

Chikungunya
- Chikungunya is a viral disease caused by the Chikungunya virus, and is transmitted by the Tigered mosquito, Aedes.
- Symptoms of chikungunya include fever, chills, severe small and large joint pains that can last for weeks and in some cases persisting for several months or years.
- A few cases of eye, neurological and heart complications along with gastrointestinal complaints have been reported.
- Serious complications are not common but, very rarely in older people, where the symptoms are mild can lead to death as the infection goes unrecognized or misdiagnosed in areas where dengue occurs.
- There is no specific treatment for Chikungunya. Symptomatic or supportive treatment basically comprises rest and use of paracetamol to relieve fever, plenty of fluids, and avoidance of aspirin.

Japanese Encephalitis
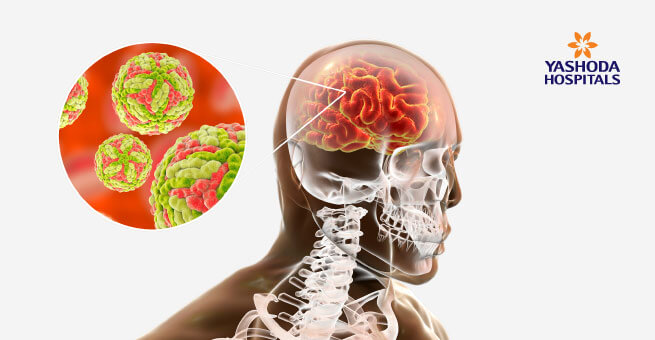
- Japanese Encephalitis virus, the causative agent of Japanese encephalitis (JE) is transmitted to humans through the bite of infected Culex mosquitoes.
- Most human infections are asymptomatic or result in only mild symptoms such as fever, headache and weakness. However, a small percentage of infected people rapidly progress to a stage of inflammation of the brain (encephalitis), with symptoms including sudden onset of headache, high grade fever, vomiting, inability to speak, disorientation, tremors and convulsions.
- One quarter of severe cases can be fatal, and 30% of those who survive severe infection have lasting central nervous system damage.
- Danger signs warranting immediate attention include unconsciousness, seizures, poor respiration and paralysis.
- There is no specific treatment for the disease. Supportive care and management of complications can provide some relief, which includes sponging for fever, paracetamol, drugs for seizure, and oxygen therapy.
- The vaccine against this disease is the single most effective preventive measure.
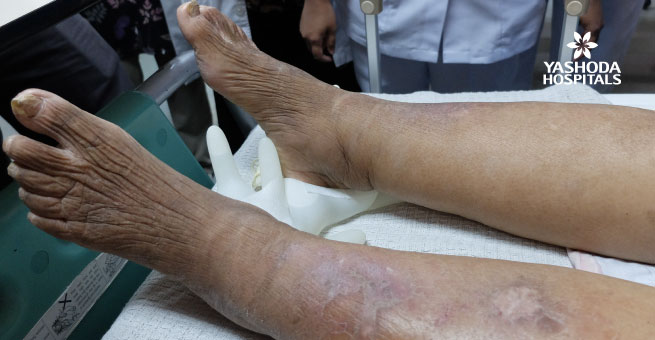
Lymphatic Filariasis
- Lymphatic filariasis, also known as elephantiasis, occurs when threadlike, filarial parasites are transmitted to humans through mosquitoes.
- The microscopic parasitic worms then lodge in the lymphatic system and disrupt the immune system. The parasites live for about 6–8 years and, during their lifetime they produce millions of microfilariae (tiny larvae) that circulate in the blood.
- The majority of infections have no symptoms but keep on silently causing damage to the lymphatic system as well as alter the body’s immune system.
- Acute episodes of local inflammation involving skin, lymph nodes and lymphatic vessels often occur and are accompanied by chronic lymphoedema (tissue swelling).
- Infection usually occurs in childhood, but the worst symptoms of chronic disease usually appear later in life – in men more often than in women – and include damage to the lymphatic system, arms, legs or genitals. It causes significant pain, and contributes to loss of productivity and social exclusion.
- Oral medications for short courses are recommended for the treatment to clear the parasites from the bloodstream. Severe lymphoedema and acute inflammation can be improved by observing strict hygiene, skin care, exercise and elevation of affected limbs. Hydrocele (fluid accumulation in the genitals) can be cured with surgery.
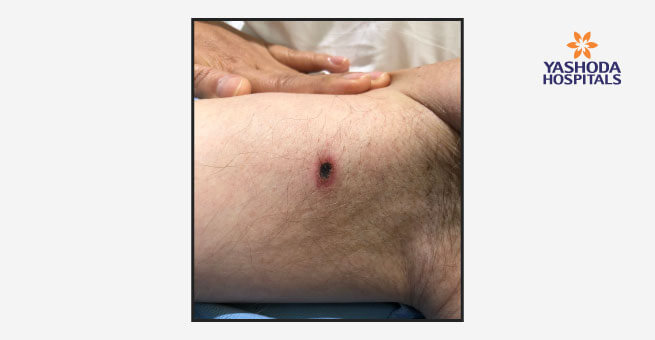
Leishmaniasis (Kala-azar)
- There are three main forms of leishmaniasis – Visceral (often known as kala-azar and the most serious form of the disease), Cutaneous (the most common) and Mucocutaneous.
- Depending on the type of leishmaniasis, the disease shows symptoms like fever, weight loss, enlargement of the spleen and liver, anaemia, rash and skin ulcers. Both cutaneous and mucocutaneous leishmaniasis can lead to disfiguring scars and are associated with stigma.
- Early diagnosis and treatment with various medications reduces the spread of the disease and can prevent disabilities and death.
Scrub Typhus
- Scrub Typhus is caused by bacteria (Orientia tsutsugamushi), and spread by bite of infected chiggers (larvae of mites).
- The most common symptoms include fever, chills, headache, body aches, rash and in severe cases can cause mental changes including confusion and coma.
- Scrub typhus is treatable with antibiotics, but they should be administered early in the course of the disease.
How can the spread of Vector Borne diseases be prevented?
Vector borne diseases can be prevented by reducing the sources where mosquito breeds. It can be achieved by:-
- Cleaning the blocked drains
- Avoiding water logging during rainfalls
- Emptying stagnant water bodies (water accumulated in old tyres, small pots and pans, coolers, small puddles at construction sites)
- Keeping water tanks and containers tightly covered
- Pouring oil over the water sources
- Introduction of larva eating fish into the water bodies
- Using insecticidal sprays in all areas of the house like DDT
- Malathion at least once a week
Personal protection from the bites of the vectors is also essential, which can be achieved by wearing clothes which cover the body as much as possible, using mosquito nets, and mosquito repellents such as sprays, creams, coils and liquids.
Rise of Vector borne diseases and their complexities amidst Covid-19
This is the time when the monsoon is at the verge of commencement and India’s health system is already over-burdened with the surge of COVID-19 and black fungus cases. This is a time when the cases of vector-borne diseases could become rampant and neglecting the preventive control measures could lead to the spike in these diseases. There should also be increased preparedness to tackle the outbreaks of vector-borne diseases during the pandemic of COVID-19, as there are high chances for the outbreak of these diseases. The vector control efforts should be in place as it is important that the COVID-19 response does not increase the vector-borne disease threats in the communities already stricken hard by the COVID-19.
References
- Climate change and threat of vector-borne diseases in India: are we prepared? PubMed: https://pubmed.ncbi.nlm.nih.gov/20155369/
- Vector-Borne Diseases, NCBI: https://www.ncbi.nlm.nih.gov/books/NBK52945/#:~:text=Population%20growth%20has%20been%20a,of%20vector%2Dborne%20infectious%20diseases.
- Vector-Borne Diseases, Mayo Clinic: https://news.mayocliniclabs.com/infectious-disease/vector-borne-diseases/
- Diseases Spread by Mosquitoes, WebMD: https://www.webmd.com/skin-problems-and-treatments/ss/slideshow-mosquito-borne-diseases#:~:text=West%20Nile,infections%20called%20encephalitis%20or%20meningitis.
- Vector-Borne Diseases in the Tropics, Johns Hopkins: https://www.jhsph.edu/courses/course/31608/2021/223.684.11/vector-borne-diseases-in-the-tropics
- Vector-borne diseases, WHO: https://www.who.int/news-room/fact-sheets/detail/vector-borne-diseases
About Author –
Dr. Monalisa Sahu, Consultant Infectious Diseases, Yashoda Hospital, Hyderabad
MD (AIIMS), DM infectious diseases ( AIIMS)

















 Appointment
Appointment Call
Call More
More