All You Need to Know about Mucormycosis

1. Why does Mucormycosis happen?
2. Why are there increased cases of infection in this wave?
3. Who is at risk for this? What symptoms should patients look out for?
4. What are the treatment options? Does it need hospital admission?
5. Who should a patient reach out to, a specialist or a general physician?
Why does Mucormycosis happen?
The Zygomycoses group of fungi, also referred to as the Mucormycosis, currently being commonly known as the black fungi, have been known to cause invasive diseases for many decades. They are present extensively in the environment and the soil. They cause diseases in the people with uncontrolled diabetes, on immunosuppressants, immunocompromised people, people on long term steroids.
With the ongoing pandemic of COVID-19, there has been a marked increase in the cases of Mucormycosis.
Why are there increased cases of infection in this wave?
The cases of Mucormycosis have increased manifold in the current ongoing second wave. Several of these cases are referred to our centre with Mucormycosis symptoms, from different regions of the twin states and also the neighboring states of Maharashtra, Karnataka and Gujarat.
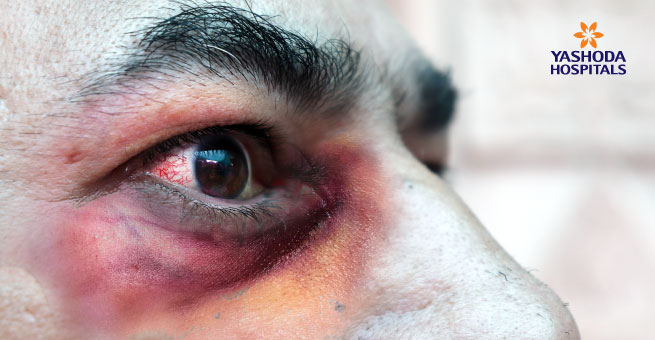
Who is at risk for this? What symptoms should patients look out for?
The COVID-19 patients with uncontrolled diabetes and diabetic ketoacidosis, those who have received high doses of intravenous or oral steroids for prolonged periods, or those who have received immunomodulators are at increased risk of the disease.
Patients with COVID-19 illness, active/recovering/post-discharge should look for the following signs and symptoms:
- Rhino-orbito-cerebral mucormycosis: nasal blockade or congestion, blackish or bloody nasal discharge; facial pain, numbness or swelling; headache or pain in the eyes and orbit; toothache, loosening of tooth or jaw involvement; blurring or double vision with pain; tingling sensation on face; fever, and blackish skin lesions.
- Pulmonary mucormycosis: Fever, cough, chest pain, blood in sputum after cough, worsening respiratory symptoms.
What are the treatment options? Does it need hospital admission?
The most common type of Mucormycosis is rhino-orbito-cerebral mucormycosis, comprising around 70-75% of the cases, pulmonary Mucormycosis seen in 15-20% of the cases and rarely gastrointestinal Mucormycosis has also been detected.
The cases of Mucormycosis have been presenting to us as early as 8-10 days after detection of COVID-19 in a few cases, to as late as about 60 days after COVID detection, the most crucial period being 2-6weeks after detection of COVID.
- Cases of Mucormycosis are to be treated as a fungal emergency (medical and surgical emergency).
- All of the presentations of the disease require aggressive management, including extensive surgical debridement of the involved tissue along with intravenous antifungals followed by oral antifungals for a period of at least 6 weeks to 3 months.
- The antifungals being used to manage the disease include liposomal Amphotericin B, isavuconazole, posaconazole and Amphotericin B deoxycholate.
Who should a patient reach out to, a specialist or a general physician?
The patient should reach out to a specialist as soon as possible because the disease requires aggressive management. A multi-disciplinary approach, including specialized surgeons like neurosurgeon, ENT surgeon, CTVS surgeon, Maxillofacial surgeon and medicine specialists including Infectious diseases physician, Neurologist, medicine specialist are required. Going to a General Physician, who may not be much aware of the signs and symptoms of the disease and if at all aware, will not be able to manage the disease appropriately and the patient will lose the crucial window period of appropriate management, as every hour in the disease counts in its management.
References:
- Mucormycosis, CDC: https://www.cdc.gov/fungal/diseases/mucormycosis/index.html
- Mucormycosis: What to Know, WebMD: https://www.webmd.com/lung/mucormycosis-black-fungus-infection
- Mucormycosis, Medicine Net: https://www.medicinenet.com/mucormycosis/article.htm
- Mucormycosis, Healthline: https://www.healthline.com/health/mucormycosis
- Mucormycosis, Medlineplus: https://medlineplus.gov/ency/article/000649.htm
About Author –
Dr. Monalisa Sahu, Consultant Infectious Diseases, Yashoda Hospital, Hyderabad
MD (AIIMS), DM infectious diseases ( AIIMS)













 Appointment
Appointment Call
Call More
More