MR Linac: A Beacon of Hope for Cancer Patients
In the world of modern medicine, technological advancements continue to push the boundaries of what is possible. One such groundbreaking innovation in radiation therapy is the integration of Magnetic Resonance Imaging (MRI) with Linear Accelerators (LINACs), commonly known as MR Linac. This remarkable fusion of imaging and treatment technologies has paved the way for a new era in precision medicine and holds tremendous promise for revolutionizing cancer care. In this blog, we will learn about the significance of MR Linac, exploring its applications, unique features, and the transformative impact it promises in the field of radiation oncology.
Need for MR Linac
The field of radiation therapy has evolved over the years, from using basic X-rays to more advanced techniques. It progressed from 2D radiotherapy to 3D radiotherapy. In the mid-1990s, Intensity Modulated Radiotherapy (IMRT) brought a significant breakthrough, setting a new standard for precision.
Further improvements led to the integration of linear accelerators with Cone Beam Computed Tomography (CBCT) in the early 2000s, paving the way for Image-Guided Radiotherapy (IGRT). While this was a crucial step, it had its limitations, such as lower soft-tissue contrast in images and the lack of real-time imaging.
To address these limitations and meet the increasing demands for precise radiotherapy, MR LINACs were introduced.
What is MR Linac?
An MR Linac is a cutting-edge medical device used in radiation therapy that combines two essential components: a linear accelerator (LINAC) and a magnetic resonance imaging (MRI) system. This integration allows for real-time, high-quality imaging during radiation treatment, providing superior precision and accuracy.
The primary advantage of the MR Linac is its ability to deliver radiation therapy with exceptional accuracy while continuously visualizing the patient’s anatomy through the MRI. This real-time imaging capability ensures that the radiation beams are accurately targeted at the tumor while minimizing exposure to surrounding healthy tissues. Furthermore, MR LINACs are particularly useful for treating tumors in areas of the body that move during breathing or bodily functions, such as the lungs or the abdomen.
In essence, an MR Linac revolutionizes radiation therapy by combining radiation delivery with live MRI imaging, significantly improving treatment precision and patient safety.
Why is MRI integrated into LINACs?
The integration of MRI into LINACs serves a crucial purpose. MRI provides exceptional soft-tissue contrast, enabling more precise differentiation between tumors and surrounding structures. This enhances the accuracy of defining treatment target areas and the critical organs at risk (OARs), which are normal organs.
In addition to its superior soft-tissue contrast, the shift toward MRI-guided radiotherapy results from several advantages MRI offers over other imaging methods:
- Radiation-Free Imaging: MRI does not use ionizing radiation, eliminating concerns about radiation exposure during multiple scans in radiotherapy.
- Versatile Imaging Sequences: MRI offers various imaging sequences that provide multiple types of information.
- Flexible Imaging Planes: MRI is not limited to specific planes like other imaging methods, making it more versatile.
- Functional and Quantitative Insights: Functional MRI and quantitative MRI techniques provide insights into the biological characteristics of tumors and surrounding tissues.
These MRI capabilities effectively address the limitations of LINACs integrated with CBCT and fully meet the stringent requirements of precision radiotherapy.
Approximately 50% to 60% of cancer patients need radiation therapy during their cancer treatment journey, either for curative (radical and adjuvant) or palliative treatments. Traditionally, imaging and radiation delivery are separate processes. Patients undergo external imaging procedures like CT scans, offline MRIs, or PET-CT scans to collect image data, which is then used to create treatment plans. Conventional LINACs deliver radiation based on pre-planned treatments without real-time adjustments. LINACs integrated with CBCT produce additional radiation during treatment verification scans. MR LINACs offer a substantial advantage by eliminating this additional radiation exposure during radiotherapy, thanks to their integrated MRI capabilities.
Did you know that MR Linac significantly reduces radiation therapy toxicity and has fewer side effects?
Distinctive Aspects of MR Linac
The primary focus of MR Linac (MRL) revolves around the identification of tumors and normal structures with the utmost precision. It achieves this through dynamic treatment adjustments that respond to changes in tumor position, body contours, and even normal organs. These adjustments happen in real time, using comprehensive motion management and live MRI during radiation therapy.
MR Linac is equipped with various distinctive aspects that contribute to its effectiveness. They include the following:
- Precision in Tissue Definition: It excels at defining soft tissues and locating tumors and normal structures with accuracy.
- Adaptive Radiotherapy: Using Adapt-To-Position and Adapt-To-Shape techniques, MRL dynamically shapes and carries out the daily treatment plan in real time, eliminating the need for repeated CT scans.
- Accounting for Body Changes: It accommodates shifts like weight loss, edema, tumor size reduction, and changes in the position of healthy organs.
- Reducing Side Effects: Precise tumor targeting helps minimize the impact of radiation.
- Real-Time Imaging: MRL employs a 1.5 Tesla MRI for real-time imaging and tracking of anatomical structures.
- Comprehensive Motion Management: It adjusts radiation delivery with high precision for organs that move with respiration or dynamic filling, such as the urinary bladder and rectum.
- Biological Adaptation: Functional MRI techniques permit dose escalation for radio-resistant tumors, simultaneous integrated boost (SIB) for specific tumor areas, and response assessment using MRI-derived biomarkers.
- SMART Approach: Stereotactic MR-guided Adaptive Radiotherapy reduces treatment side effects while enhancing outcomes and quality of life.
Workflow of MR Linac
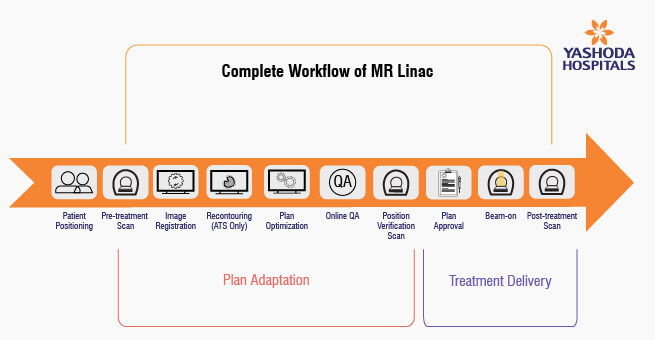
Patient Positioning: The process begins with carefully positioning the patient in the MR Linac for the radiation therapy session.
PLAN ADAPTATION:
- Pre-treatment Scan: Before treatment, a scan is performed to capture images of the patient’s anatomy.
- Image Registration: The images obtained from the scan are registered and aligned with the treatment plan.
- Recontouring (ATS only): In cases where Adapt-To-Shape (ATS) is utilized, recontouring is done, ensuring that the treatment plan matches the patient’s current anatomy.
- Plan Optimization: The treatment plan is optimized to adapt to the patient’s specific anatomy and needs.
- Online QA: Quality assurance checks are performed to ensure that the treatment plan is accurate.
- Position Verification Scan: Another scan is conducted to verify that the patient is correctly positioned for treatment.
TREATMENT DELIVERY:
- Plan Approval: The treatment plan is reviewed and approved.
- Beam-on: The radiation beam is activated for treatment.
- Post-treatment Scan: After treatment, a final scan may be performed to assess the accuracy of the treatment delivery.
This workflow ensures that each step is executed with precision, allowing for real-time adjustments to optimize treatment and enhance patient safety and outcomes.
With its unparalleled precision, real-time adaptability, and the ability to minimize radiation exposure, MR Linac is transforming the landscape of radiation therapy and ushering in an era where personalized, effective, and safer cancer treatments are a reality.
https://youtu.be/aphkJJNW2Tw?si=vBQAHmSnq26A__IS
References:
- MRI-guided Radiation Therapy: An Emerging Paradigm in Adaptive Radiation Oncology
https://pubmed.ncbi.nlm.nih.gov/33350894/ - Emergence of MR-Linac in Radiation Oncology: Successes and Challenges of Riding on the MRgRT Bandwagon
https://doi.org/10.3390/jcm11175136 - Advances in MRI-guided precision radiotherapy
https://doi.org/10.1002/pro6.1143 - Assessment of planning target volume margins in 1.5 T magnetic resonance-guided stereotactic body radiation therapy for localized prostate cancer
https://doi.org/10.1002/pro6.1155














 Appointment
Appointment Call
Call More
More