Managing Mumps: Symptoms, Treatment, and Prevention

An unexpected mumps outbreak has caused chaos among the populace, with a surge in cases reported across multiple Indian states. According to government data as of March 2024, there have been 15,637 reported cases this year.
Mumps disease is a highly contagious viral infection primarily affecting the salivary glands, notably the parotid glands beneath the ears. It spreads through respiratory droplets when infected individuals cough or sneeze, leading to complications such as testicular or ovarian inflammation, meningitis, and potential deafness.
Children who are unvaccinated and between the ages of 2 and 12 are most usually affected by mumps. Even after receiving a vaccination to prevent it, adults and teenagers can still contract the mumps. This happens because, after a few years, the vaccine’s immunity wanes. Being completely vaccinated remains the best defense against mumps infection, nevertheless.
Vaccination is key to preventing mumps, with both children and adults advised to receive recommended doses. Practicing good hygiene, including frequent handwashing, avoiding close contact with infected persons, and covering the mouth and nose when coughing or sneezing, also aids in prevention. Swift identification of symptoms and isolation of infected individuals are crucial preventive measures.
Is Mumps Contagious?
Mumps is caused by a virus that spreads through respiratory droplets expelled when an infected person coughs, sneezes, or talks. The virus can also spread through contact with items people use, such as straws, drinking glasses, and soiled tissues. Any surface they come into contact with can transmit the mumps to other people if they don’t wash their hands.
It’s possible for mumps to be contagious before swelling appears and for up to 5 days after swelling begins. When the mumps is at its most contagious, it lasts for two days before symptoms appear and for several days after they do. Even those without symptoms can spread the illness to others who are sick.
Mumps Signs and Symptoms
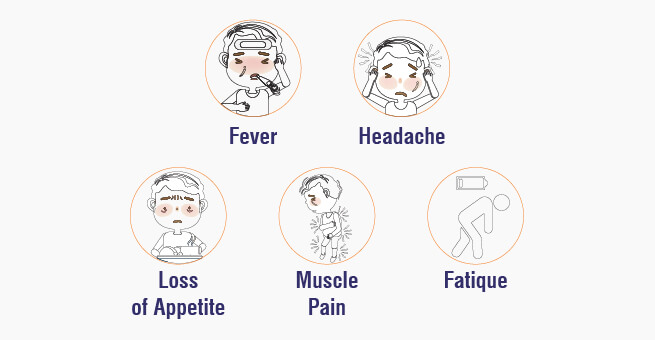
Symptoms typically appear 2 to 3 weeks following exposure to the virus, with an incubation period ranging from 2 to 3 weeks. While some individuals may exhibit no symptoms or experience only mild ones, others may develop flu-like symptoms initially, including fever, headache, muscle aches, loss of appetite, and fatigue.
Within a few days, swelling of the salivary glands becomes apparent, often affecting one or both glands on the sides of the face. This swelling may be accompanied by pain or tenderness around the affected areas. In rare cases, glands below the floor of the mouth may also swell. Diagnosis can be challenging due to mild or absent symptoms, underscoring the importance of early recognition and isolating infected individuals to prevent transmission.
Some cases may develop complications like testicles pain & swelling in males & ovaries inflammation (oophoritis) in females. Severe complications include pancreatitis or meningitis.
Prevalence of Mumps in Adults
Adults can also contract mumps, although it’s less common due to widespread vaccination. However, adults who haven’t been vaccinated or haven’t had mumps in the past are still at risk. Mumps in adults can lead to more severe complications compared to children, including inflammation of the testicles, ovaries, or pancreatitis,meningitis, and, in rare cases, hearing loss or miscarriage in pregnant women.
Symptoms in adults are similar to those in children and may include fever, headache, muscle aches, fatigue, and swelling of the salivary glands. Treatment typically involves rest, fluids, and pain relievers to alleviate symptoms, and isolation to prevent the spread of the virus to others.
How long does mumps last?
Mumps typically lasts for about 7 to 10 days, with symptoms starting to appear around 10 to 14 days after exposure to the virus. Fever may continue for 3 to 4 days, while swelling of the parotid glands, if present, usually lasts for about 7 to 10 days. It’s worth noting that up to one third of individuals infected with mumps may experience very mild or no symptoms at all.
Mumps complications are more prevalent in adults than in children and may include:
- Meningitis or encephalitis: Inflammation of the membrane covering the brain and spinal cord or inflammation of the brain, which can lead to severe consequences like seizures, stroke, or even death.
- Orchitis: Inflammation and swelling of one or both testicles, potentially impacting sperm production. In rare cases, it may lead to sterility.
- Mastitis: Inflammation of breast tissue.
- Parotitis: Inflammation and swelling of one or both parotid glands located on the face, in front of the ears.
- Oophoritis: Inflammation of one or both ovaries, which, in rare instances, can hinder fertility.
- Pancreatitis: Inflammation of the pancreas.
- Deafness: Mumps can result in hearing loss.
While there have been reported instances of nephritis, myocarditis, and other rare complications like paralysis, seizures, cranial nerve palsies, and hydrocephalus in mumps patients, these occurrences are extremely rare. Death from mumps is exceedingly uncommon.
Is Mumps curable?
While there is presently no cure for mumps, the infection typically resolves within 1 or 2 weeks. Treatment focuses on alleviating symptoms and includes:
- Resting in bed and ensuring an adequate intake of fluids.
- Using painkillers to manage discomfort.
To diagnose mumps, your healthcare provider will assess your symptoms and inquire about any recent exposure to individuals with the infection. If mumps is suspected, a sample may be collected, either by swabbing the mouth or gathering urine, to test for the presence of the mumps virus. Additionally, a blood test will be conducted to detect antibodies produced by your body in response to the virus, aiding in confirming the diagnosis.
Mumps treatment typically involves pain relief medication and ample fluid intake. Bed rest may be necessary, especially during the initial days of the illness. Adults should refrain from work for at least 5 days after the onset of gland swelling, while children should remain out of school until symptoms subside. Both adults and children displaying mumps symptoms should minimize contact with household members. Practicing good hygiene, such as frequent handwashing, covering the mouth when sneezing or coughing, and regularly sanitizing commonly touched surfaces, is crucial for disease control.
Mumps prevention
Mumps is highly preventable thanks to the effectiveness of the mumps vaccine, typically administered as part of the measles, mumps, and rubella (MMR) combination vaccine. Children typically receive two doses of the MMR vaccine according to the childhood immunization schedule: the first dose between 12 and 15 months of age, and the second dose between 4 and 6 years old. While mumps cases are rare, vaccinating your child is crucial to minimizing their risk, particularly in light of recent outbreaks. In outbreak situations, public health authorities may recommend a third dose of the mumps vaccine for affected individuals.
The MMR vaccine is highly safe and effective, preventing mumps in up to 90% of individuals. Most children experience no side effects from the vaccine, and any that do occur are typically mild. These may include a rash, fever, or slight discomfort at the injection site.
While extremely rare, some children may have an allergic reaction to the MMR vaccine. If your child experiences difficulty breathing, fatigue, loss of color, or wheezing after vaccination, seek immediate medical attention from their healthcare provider.
Children with minor illnesses, such as mild respiratory infections or low-grade fever, can still receive the vaccine. However, if your child has a more serious illness, their pediatrician may recommend delaying vaccination until they have fully recovered.
About Author –

















 Appointment
Appointment Call
Call More
More