Bladder cancer and its treatments
At a Glance:
2. What are the types of bladder cancer?
3. What causes bladder cancer?
4. What are the symptoms of bladder cancer?
5. How is the bladder cancer diagnosed?
6. What is the treatment for bladder cancer?
7. What are the other modalities of treatment for MIBC?
What is bladder cancer?
Bladder cancer is an abnormal growth of cancer cells in a person’s urinary bladder. The disease presents as one or more lumps in the urinary bladder.
What are the types of bladder cancer?
Bladder cancer is basically of two types-
- Non-muscle invasive bladder cancer: In this type, the cancerous growth involves the thinner inner surface of the bladder. The bladder muscle is not involved and hence the name. The tumour does not spread outside the bladder and there are several treatment options available for this disease which has got good prognosis.
- Muscle-invasive bladder cancer: Muscle invasive bladder cancer spreads into the thick muscle deep in the bladder wall. It is a serious and an advanced disease which needs immediate treatment.
What causes bladder cancer?
Smoking is the most important cause of bladder cancer. Tobacco consumption in any form predisposes to cancer. Exposure to certain chemicals used in plastic, rubber, leather and paint industries can also trigger bladder cancer. Prior treatment with radiation and chemotherapy drugs like cyclophosphamide also can lead to the disease.
What are the symptoms of bladder cancer?
Bladder cancer at times can progress without causing any symptoms. But one should consult a urologist if any of the following symptoms are seen.
- Hematuria – blood in the urine, usually it is painless
- Irritative urinary symptoms like frequent urination, urgency.
- Lower abdominal pain and back pain.
How is the bladder cancer diagnosed?
Your doctor after history and physical examination will confirm the disease by ordering the following investigations.
- Complete urine examination to see for hematuria
- Urine for malignant cytology to look for cancer cells in urine
- Ultrasound of abdomen and pelvis
- Renal function tests
- CT scan of abdomen and pelvis.
- Cystoscopy: endoscopic examination of the bladder
What is the treatment for bladder cancer?
The treatment depends on the stage and the grade of the cancer. Tumours which appear to be confined to the inner surface of the bladder wall are removed completely by an endoscopic technique called – TURBT – Transurethral resection of bladder tumour. In TURBT a resectoscope is passed through the urine passage into the bladder and the tumour is resected by electrocautery.
The resected tumour tissue is sent for histopathological examination to know the grade and whether the tumour is non-muscle invasive or muscle invasive.
Non-muscle invasive bladder cancer (NMIBC):
NMIBC type of bladder cancer is completely removed by TURBT which is both a diagnostic and therapeutic procedure in these patients. Certain types of non-muscle invasive bladder cancer need intravesical immunotherapy or chemotherapy to completely eradicate the disease and to prevent recurrence.
Intravesical BCG (Yes ! it is the same vaccine we take to prevent tuberculosis disease) is the commonly used immunotherapeutic agent. BCG is administered into the bladder weekly for 6 weeks with all the necessary precautions usually 4 wks after the TURBT. Intravesical Mitomycin is another commonly administered chemotherapy drug to prevent recurrence.
Muscle-invasive bladder cancer (MIBC):
The treatment depends on stage of the disease. Staging is done by TNM staging system. MIBC confined to the bladder can be cured by complete surgical removal of the bladder. The operation is called radical cystectomy.
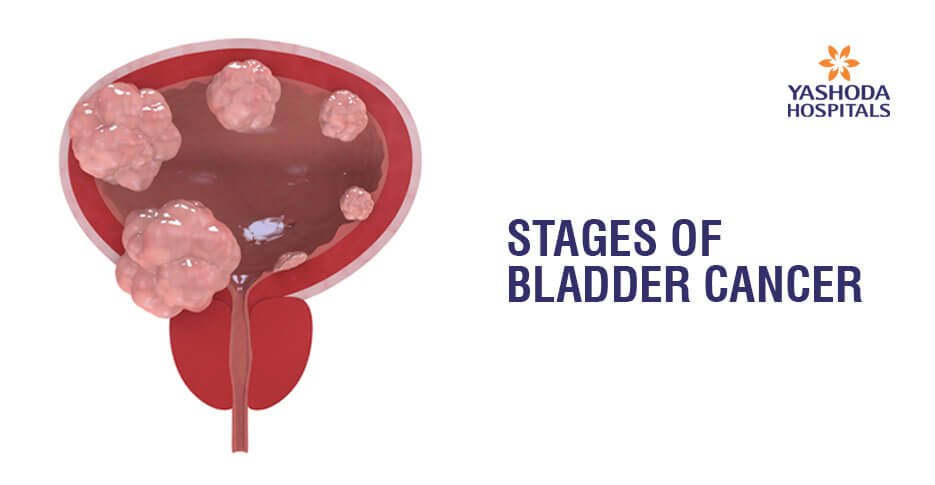
In men, entire bladder along with the prostate, seminal vesicles and lymph nodes are removed. In women, part of the vagina and sometimes the uterus is also removed along with the bladder.
When the bladder is removed urinary diversion operation is done for the urine excretion. There are 3 types of urinary diversion operative procedures. In the simplest type called urinary conduits, both the ureters from the kidneys are joined to a small isolated intestinal segment which is brought out to the body as a stoma. The patient has to wear an appliance to collect the continuously leaking urine.
The second type of urinary diversion is the continent diversion. In this operation, the urine is diverted either into rectum or into a continent cutaneous pouch. In rectal urinary diversions, patient passes urine and stools through the anus. In continent cutaneous diversions, the urine collected in the pouch is let out by regularly self emptying the pouch with the soft catheters. There is no need to wear an appliance after this operation.
The third type of urinary diversion is the orthotopic urinary bladder. In this operation a neobladder is created with a long segment of intestine. The new bladder is connected to the normal urine passage. This technically demanding operation allows the patient to pass urine normally.
In patients with locally advanced disease , chemotherapy is given before the surgery to downsize the tumour and make it operable.
What are the other modalities of treatment for MIBC?
Radiotherapy is another modality of treatment for MIBC. Radiation is usually given for patients not fit for surgery and who want to preserve the bladder.
Can the bladder cancer recur after the treatment ?
Bladder cancer is notorious for recurrence. Hence patients need to be on regular follow-up.
NMIBC can recur in the future and may also progress to MIBC. MIBC patients after bladder removal can develop recurrence in other regions of the body.
How is the follow-up done for bladder cancer patients?
The follow-up is different for NMIBC and MIBC tumours.
In NMIBC, follow-up depends on risk category. For low risk patients, a cystoscopy is done 3 months after TURBT. For intermediate risk group, urine cytology and cystoscopy are done every 3 months in the first year, every 3-6 months in the next 2 years and every year thereafter. High risk patients need a more frequent cytology and cystoscopy examination. Follow-up is lifelong in intermediate and high risk groups.
MIBC patients who have undergone bladder removal are advised blood tests, CT scan of the abdomen to see for any recurrence.
About Author –
Dr. V. Surya Prakash ,Consultant Urologist, Laparoscopic, Robotic & Transplant Surgeon
MS (Gen Surgery), FRCSED, M.Ch(Urology), DNB(Urology), D.Lap

















 Appointment
Appointment Call
Call More
More