Coronary angioplasty with rotablation in elderly
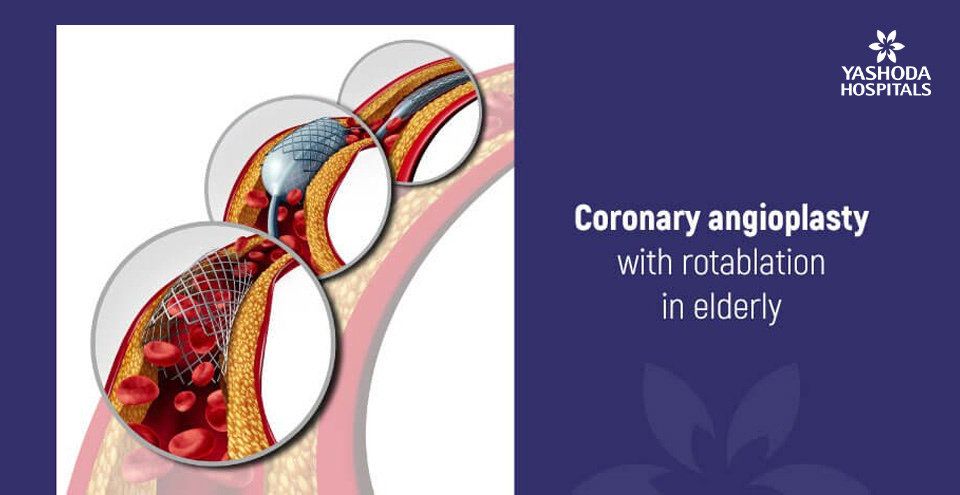
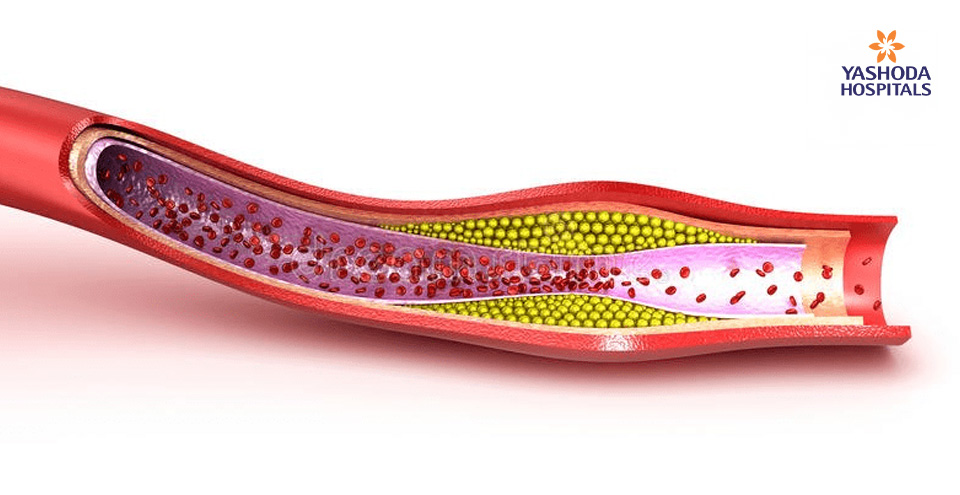
Angioplasty is performed more often as it is a percutaneous procedure and a safer option to remove blockages formed in arteries [Coronary] of the heart. When the patient is above 80 years, the procedure becomes technically difficult because of age-related changes that occur in the body. As the age advances the arteries become harder due to the patho-physiological process of atherosclerosis. This process leads to deposition of calcium in the arterial wall making them harder as compared to the arteries of younger patients. The calcium deposits over the blockage from inside the lumen of the vessel and also on the outer wall of the vessel.
The angiography of the coronary arteries might reveal complete occlusion in elderly who presented without any symptoms. This is because they develop blocks over a period of time and the blocked vessel develops smaller channels called collaterals, which tend to grow in size and number as time passes.
While the blockages in the younger individuals are easy to dilate using the balloon, owing to the softer nature of the block, it is less likely to remove the blockages with similar ease in the elderly. These blocks are relatively difficult to negotiate because of a hard matrix containing calcium and other natural salts in addition to fat. The harder blocks, which cannot be dilated using balloon before deployment of the stent due to calcium deposition, need Rotablation, an interventional tool for debulking the harder lesions.

Rotablator burr: A special catheter, with an acorn-shaped, diamond-coated tip, is guided to the point of narrowing in your coronary artery. The tip spins around at a high speed and grinds away the plaque on your artery walls
For the elderly, angioplasty is palliative care (treatment for relieving pain without dealing with the cause of the condition) and should be done as a lifesaving procedure to prolong the life of the patient. The mathematics of blocks is not simple. For some people with multiple blocked vessels, doctors may advise only lifestyle modifications and medical management in the form of oral pills that keep blood thin and keep cholesterol low(statins). The medical management is a good option in cases where a complicated angioplasty procedure is suspected to compromise the chance of survival further. But the decision has to be made after a thorough evaluation of risk with the help of risk calculators available i.e. for the risk of bleeding with the use of blood thinners [Anti-platelet and/or anticoagulant] and the risk of ischemia [means the reduction in blood flow to the heart] and cardiac death.
Some individuals who have only a single or multiple block/s may require an angioplasty or even bypass surgery. If the block is in the left main parent vessel or multiple blocks, then bypass surgery is advised. Lesser blocks can be managed by the coronary angioplasty instead of bypass surgery in the elderly (especially those above 80 years). In patients with multiple blockages and elderly patients, angioplasty of the symptoms causing blood vessel can be performed and other asymptomatic blocks (which are not causing symptoms) can be left on medical treatment.
Post-procedure there are certain rare complications such as the development of bleeding at the arterial puncture site in cases of angiography and angioplasty via femoral artery near the groin region. The reported incidence of bleeding and hematoma formation is higher with cardiac procedures from leg artery. So, I perform a majority of procedures through the hand artery which is known as Radial angioplasty, which leads to very less complication at the access site as shown in the figure below.
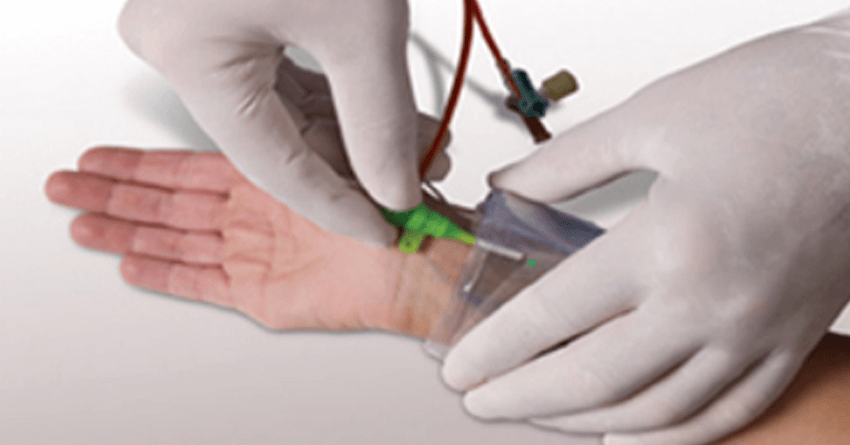
Radial Angioplasty: The image shows the removal of the radial sheath after angioplasty and application of compression using the radial compression band. This band is removed after 5-6 hours, which minimizes the access site complications like bleeding or hematoma formation.
Risks in the elderly
Stroke/paralysis: With advancing age, the aging process involves the aorta also and there is deposition of cholesterol, calcium on the walls of the aorta. During manipulation, the catheter can embolize them into the blood vessels of the brain which can lead to stroke or paralysis. However with the assistance of interventional radiologist and neuro physician round the clock and we can tackle these issues.
Bleeding: Blood-thinning medications which are called as ‘antiplatelet and anticoagulants’ are given to patients to prevent the development of the fresh clot formation at the site of angioplasty where the stent was deployed by the surgeon. This may lead to bleeding from the access site (the site where the artery was punctured) particularly, in the access sites in the groin.
But we perform Radial angioplasty, which minimizes the risk of bleeding to as low as 1%. Also, we perform snuffbox access, which reduces the risk of access site complication to the bare minimum. The ultrasound guidance gives us a proper puncture point. The team of interventional radiologist and vascular surgeon help us in planning access before the procedure and management of access site complication.
Kidney Failure: Age-related decrease in the functioning of the kidneys and the use of contrast combined can lead to elevation of serum creatinine and acute kidney failure. The improvement in the renal function is observed in most the patient but less than 1% patient may need dialysis. The use of proper hydration alleviates the problem in consultation with Nephrologist who will guide us in the management of such cases. Also, we can limit the amount of contrast used to very minimum quantity, which is nephrotoxic with help of intravascular ultrasound [IVUS] while performing angioplasty. We have round the clock Expert Nephrology services available where patients with underlying kidney disease can be managed.
My Experience in the treatment of Elderly
At Yashoda Hospitals, I have addressed many elderly patients who had a heart attack. The oldest patient I treated so far was of 95 years age, he is still surviving without any complications. Let me discuss a case where I did angioplasty for a 75-year-old gentleman who presented with recent onset effort angina on exertion for 15 days. He lived with hypertension and he was a reformed smoker. His coronary angiography revealed calcified right coronary artery [proximal to distal] with critical stenoses of distal two branches namely posterior descending artery [PDA] and postero-lateral branch [PLB]. Left coronary angiography showed mild lesion of the left anterior descending artery and osteal complete occlusion of another left-sided artery, which was blocked for a long time.
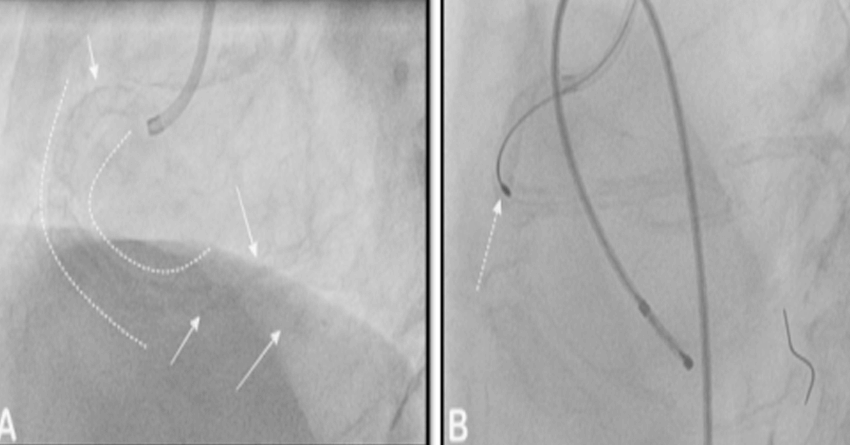
Panel A: The curved dashed lines across the entire course of the right coronary artery depicting the presence of the calcium, which posed difficulty in crossing the artery. Panel B: the use of Rotablation for debulking the calcium from the lesion. The Rota burr is seen crossing the vessel under the presence of temporary pacemaker wire as a standby if the patient develops heart blocks leading to low heart rate
To relieve his chest pain I attempted to do the angioplasty of the right coronary artery branches – PDA and PLB as described earlier. But I was facing trouble in passing the smallest size balloon due to extensive calcium in the entire course of the vessel.
Hence the use of the rotablation was advocated which modified the lesion in the artery. Then I could deliver the stent to both the branches and complete the procedure. The left-sided blockages were left on medical management and patient was discharged on the 2nd day after the procedure without any complication with the prescription of regular medications. Patient has completed more than 2 years since the procedure and he is doing very well & leading quality life without any chest pain.
The department of interventional cardiology at Yashoda Hospitals, Somajiguda has witnessed successful cases of the radial angioplasty with rotablation in the elderly patients presenting with a heart attack and/or blockages in the arteries of their heart. The risks involved in the procedure are very minimal and greatly under control so the patients return to normal life without any health risk.
Disclaimer: The content on this page is for patient education only. Please consult your doctor for a thorough investigation and an informed decision.
About Author –
Dr. Pankaj Vinod Jariwala, Consultant Interventional Cardiologist, Yashoda Hospitals – Hyderabad
MD, DNB, DNB, MNAMS, FICPS, FACC.
Fellowship in Interventional Cardiology [ICPS, Paris, France]He has performed 5000+ percutaneous trans-luminal coronary Angioplasty & 10,000+ Coronary Angiograms and treated 500+ structural heart diseases (including congenital) with Percutaneous Balloon Mitral Valvuloplasty [PBMV] and other pediatric & adult cardiac interventions.















 Appointment
Appointment Call
Call More
More