Post Covid Care: Guidelines for People Recovering Post Covid-19

INTRODUCTION
If you have just recovered from COVID-19 or returned home from the hospital, you have won the battle but the war is still on. Pat yourself and get ready for more battles as you get back to your routine life.
After recovering from acute phase of illness, It’s important to continue being cautious especially after discharge. Post COVID period needs a supervised care and persistent cautious attitude. Home quarantine should be done for appropriate duration as per your doctor.

What measures to be taken at home after discharge
- Continue COVID appropriate behaviour (use of mask, hand & respiratory hygiene, physical distancing)
- Readdress your ongoing medications for other pre-existing ailments
- Self-monitoring is essential to inform daily check of oxygen levels and temperature.
- Look for warning signs like fever, breathlessness, low oxygen levels (Sp02 < 95%), unexplained chest pain, new onset of confusion, focal bodily weakness
- If you are started on blood thinners, keep a close watch on bleeding from any site like red coloured urine, blood in stools, blood in phlegm
- If you are started on oral corticosteroids, monitor your sugar levels
- Ensure nutritious diet, adequate hydration (with plenty of fluids) and sound sleep
- Be vigilant and vocal about your mental health
- Recovered individuals should discuss the importance of right reflexes at right time and clear the myths and stigma around the disease
- Professional work to be resumed in graded manner only after confirming with treating Physician
- COVID Rehabilitation is extremely beneficial
- Advisable to follow up with Physician after 10 days from discharge
What to do for post covid Fatigue?
Fatigue is a common sign of viral infection. This is because the body diverts a lot of energy from the normal body processes to the infection. Some patients report extreme fatigue that can continue for a little while after they beat the disease.

You can try these six tips to deal with fatigue after COVID-19
- Make a new timetable with your current energy levels in mind. Plan meticulously.
- Reorganise your space/office/desk to reduce energy consumption.
- Be honest about how much you can take, and the things that need your input. Assign a priority to the tasks you set for yourself.
- Go slow: pace yourself.
- Don’t overlook how you are feeling.
-
Eat energy-boosting foods.Bananas, apples, oranges and sweet potatoes are great for getting energy quickly. You can also add a little bit of honey to warm lemon water and drink that for a quick pick-me-up. When you are feeling really low energy, sipping on water can be surprisingly helpful.
What to do if you have Cough?
Dry Cough
- Drink lots of fluids. Include warm drinks like an infusion of tulsi leaves in boiled water or honey and lemon in warm water.
- Try to avoid alcohol, sugary drinks and coffee for some time, as these can cause dehydration.
- Sip on water throughout the day-don’t gulp several glasses at a time, sip slowly and frequently.
- Suck on a throat lozenge it will keep your throat moist and bring some relief.

Cough with Sputum
- Steam inhalation can loosen the phlegm and help it to come out. Take steam twice or thrice a day, for about 15 minutes each time.
- Try sleeping on one side rather than flat on your back. You could also sleep in the high side-lying position (on one side, with your head raised on multiple pillows).
- Drink lots of fluids, including high-protein and high-energy drinks like bone broth, and vegetables and lentil soup.
- You can also drink kadha made by boiling ginger, tulsi and black pepper in water for 5-7 minutes.
What to do if you have Anxiety?
The experience of having COVID-19 can be very frightening. The experience can have an emotional impact. These will help:
- Avoid watching too much news or social media if it is making you feel anxious, try limiting yourself to looking at the news once a day
- Take up meditation or yoga to de-stress and jumpstart your physical recovery
- Stay connected with friends and family over the phone and video calls
- Find and enjoy new activities (Cooking, Gardening & Painting)

What to do if you have Chest Congestion?
Active Cycle of Breathing Technique (ACBT) Exercise
This is a multi-step breathing exercise that help to expel phlegm and chest congestion. Here’s how to do it:
- Breathing control : Gentle, relaxed breathing with your shoulders relaxed
- Deep breaths: • Breath in slowly and deeply • Gently breathe out without forcing it.• Repeat 3-4 times only (too many can make you feel dizzy)
- Forced expiration techniques (Huff): •Take a medium sized breathe in • Breathe out forcefully for a short time • Keep your mouth open and use your stomach and chest muscles • Think ‘huffing’ a mirror to polish it • Repeat 1-2 times • Always finish on a cough or huff • Stop when your huff is dry on two consecutive cycles.
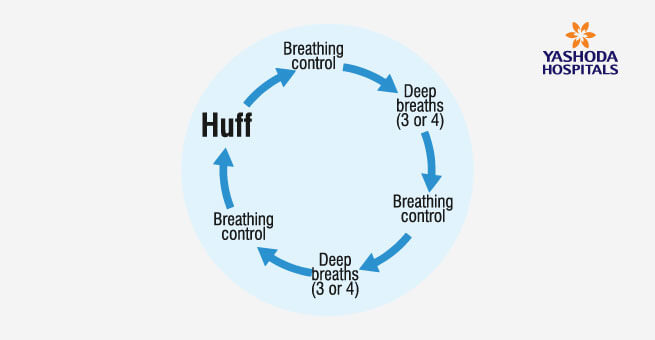
How often and how long?
- Continue to do until you feel your chest is clearer
- Perform for at least 10 minutes, but no longer than 30 minutes, Repeat 2-3 times per day
Positions to help keep your chest clear
Lie down on your right side with one or two pillows under your hips. You can also increase the number of pillows to three, and drain the lower lobes (sections) of the lungs.
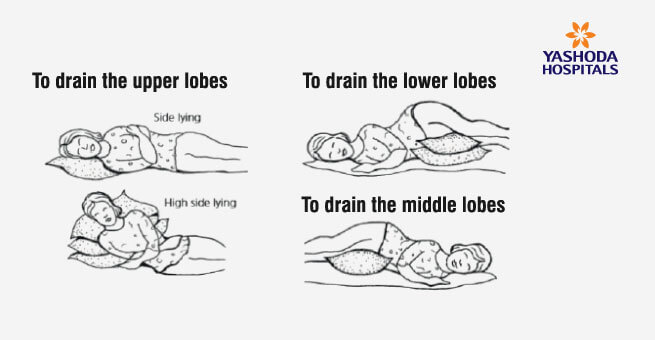
Do not do this if :
- Immediately before or after a meal
- Stop if you have any side effects
- Nausea
- Acid Reflux
- Become significantly breathless
- Have blood in your phlegm
- Have a recent chest, spine or rib injury
- Feel wheezy
Managing Shortness of Breath
When to use S.O.S. for Shortness of Breath?
- To recover after coughing.
- To recover after exercise or activity .
- To help control panic and anxiety.
- To help control sudden onset of shortness of breath.
- To aid in relaxing the breathing muscles.
Positions to ease Shortness of Breath
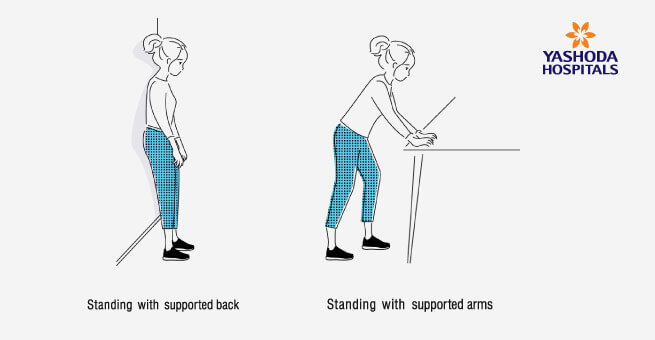
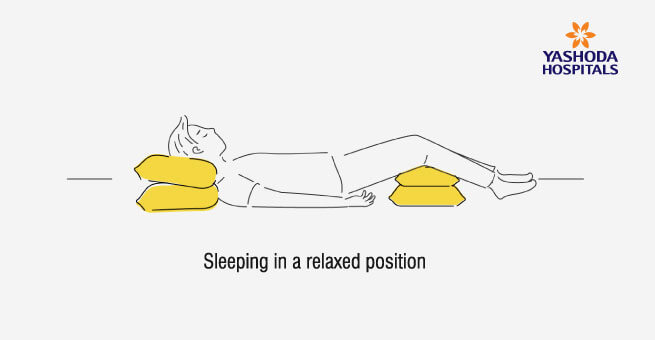
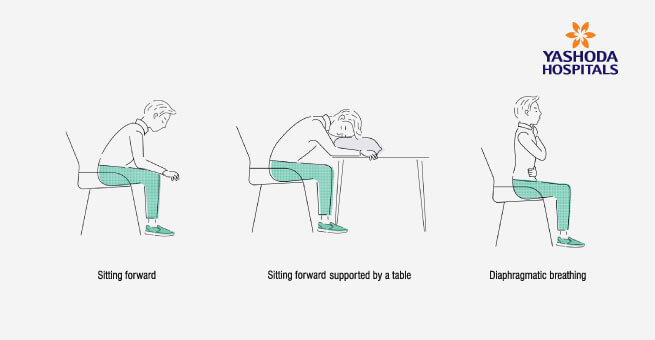
Breathing Training
Breathing training is an essential part of managing respiratory conditions as they help to clear the sticky mucus from the lungs, and keep the airways open.
What does breathing training do?
- Moves stale air and carbon dioxide out of the lungs
- Moves fresh air and oxygen into the lungs
- Helps control shortness of breath at rest and with activity
- Helps remove mucus from the lungs
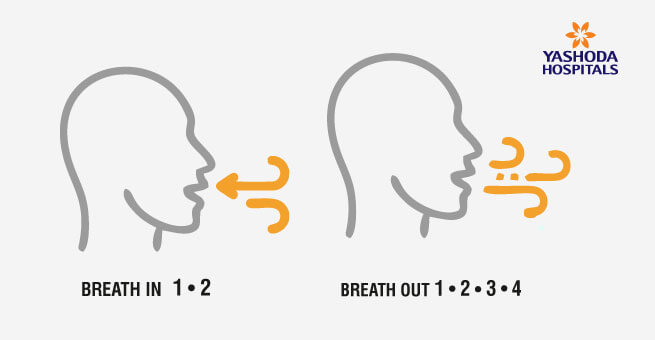
1. PURSED LIP BREATHING (PLB)
- Breathe in slowly through your nose & count 1 & 2.
- Purse your lips in a whistling position.
- Breathe out gently through pursed lips and count 1 to 4.
- Don’t force air out of your lungs.
2. DEEP OR DIAPHRAGMATIC (BELLY) BREATHING
- Lie on your back on a flat surface (or in bed) with your knees slightly bent. To make it more comfortable, you can use a pillow under your head and your knees for support.
- Place one hand on your upper chest and the other on your belly, just below your rib cage.
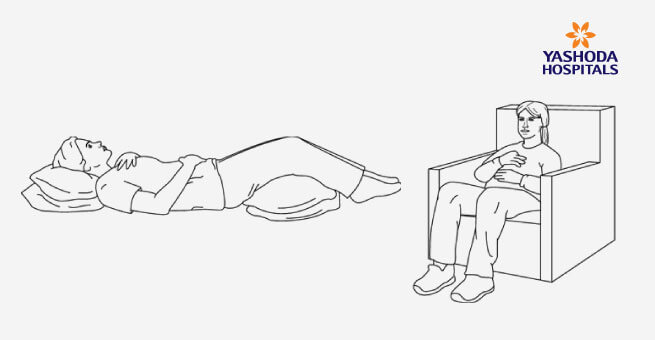
- Slowly breathe in through your nose & feel your belly rise. The hand on the chest should remain still, while the one on your belly should rise.
- Slowly breathe out through pursed lips and feel your belly fall inwards as you exhale.
- Keep your shoulders relaxed and not hunched up.
- Do this in a sitting or lying position.
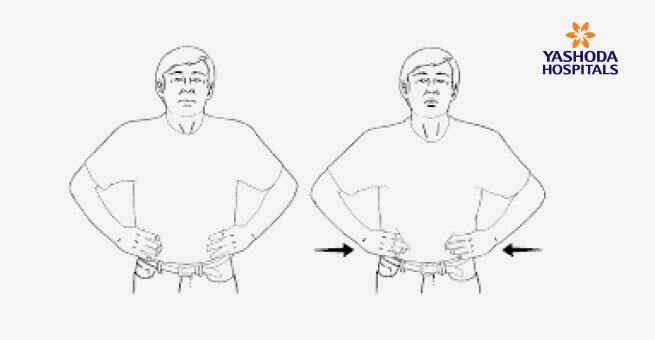
3. RIB BREATHING
- Flatten your hands on the lower part of your rib cage.
- Breathe in through your nose and feel the ribs move outward.
- Breathe out and feel your ribs flattened.
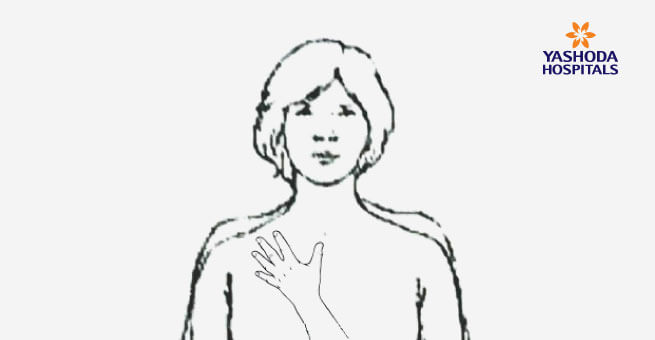
4. CLAVICULAR BREATHING
- Keep your hand just below the collar bone.
- Breathe in through your nose and feel your fingers raised.
- Breathe out and feel your fingers flattened.
NOTE
- Practice these techniques 4-5 times a day at first so you can get the correct breathing pattern correct.
- Don’t exercise immediately after taking food. Wait for an hour after taking food.
- If you cannot do it 10 times, do it according to your tolerance.
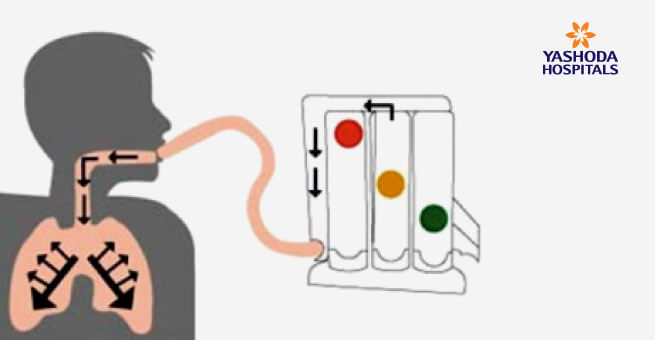
SPIROMETRY
- Sit upright in a chair or in bed.
- Put the mouthpiece in your mouth and close your lips tightly around it.
- Breathe in (inhale) slowly through your mouth.
- Hold your breath for 10 seconds, or as long as possible.
- Breathe out (exhale) deeply into the mouthpiece.
- Repeat 10 times, try to lift as many balls as you can.
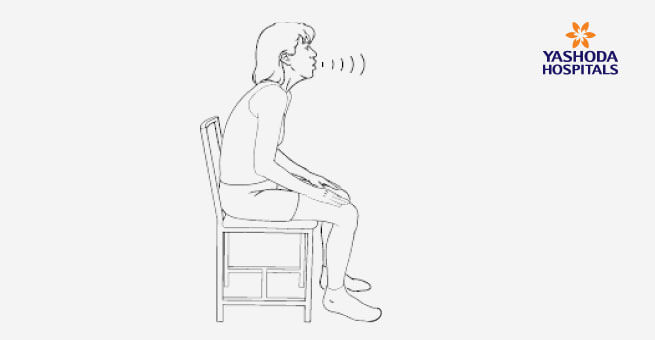
CLEARING THE AIRWAYS
- Sit up and take a slow deep breath until your lungs are almost full.
- Try to hold the deep breath for 2 -3 seconds.
- Cough 2 times with your mouth slightly open.
- Cough the mucus into a tissue.
- Discard the tissue in a closed bin.
- Wash your hands.
- Do this with your breathing exercises.
Managing problems with Attention, Memory & Thinking Clearly
It is very common for people who have been severely unwell, especially those who had a breathing tube in hospital, to experience new difficulties with attention, remembering things, and thinking clearly. These difficulties may go away within weeks or months, but for some people, they can last longer-term. It is important for you and your family to recognize if you are experiencing these difficulties, as they can have an impact on your relationships, daily activities, and your return to work or education. If you experience these difficulties, these strategies may help:
- Physical exercise can help your brain recover. While this may be difficult if you are experiencing weakness, breathlessness, or fatigue, try gradually introducing gentle exercise into your daily routine
- Brain exercises, such as new hobbies or activities, puzzles, word and number games, memory exercises, and reading may help
- Prompt yourself with lists, notes, & alerts, such as phone alarms, that can remind you of things you need to do
- Break down activities into individual steps to avoid feeling overwhelmed

Physical Exercise
If you have any kind of discomfort stop exercising and contact your healthcare professional:
WARM-UP EXERCISES:
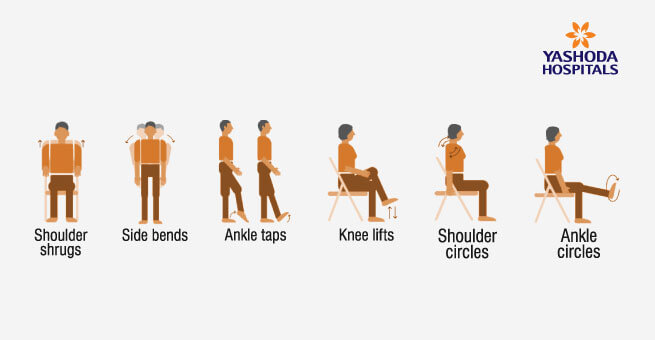
FITNESS EXERCISES : You should aim to do fitness exercise for 20-30 minutes, 5 days each week.
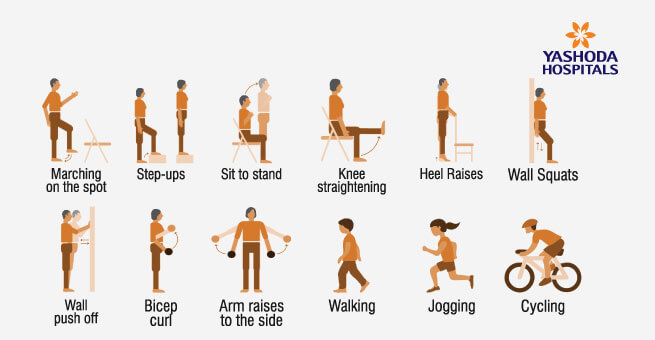
COOL DOWN EXERCISES & MUSCLE STRETCHES: Your cool down should last approx. 5 minutes. Walking at a slower pace or gently marching on the spot, for approx. 2 minutes. Stretching your muscles can help to reduce any soreness and help your joints.

Managing your Diet
You may find that your taste changes during and for a period of time following COVID-19. However it is important to eat and remain well hydrated.
Aim to have 3 hand size items from this Protein group daily
Beans, pulses, sh, eggs, meat and other proteins. Eat more beans and pulses, less red and processed meat.

Aim to have 3 thumb size items from this Dairy* group daily
*If you want to gain weight choose the full fat and full sugar versions.

How can you get enough vitamins and minerals?
Aim to have 5 handfuls from this fruit and vegetable group each dayEat with the rainbow; different colours Provide different vitamins and minerals.

Once you regain your weight and energy, switch to BALANCE DIET for a healthy life.

Post Covid-19 Complications
Some people who’ve had COVID-19 may experience multiple health complications long into the future. Covid sequelae are referred to as acute issues arising from a chronic ailment. Although COVID-19 largely affects the lungs, with the interconnected nature of the body, the study has shown Metabolic, Cardiovascular, Musculoskeletal, Rheumatological, Haematological, General and Neurological complications secondary to the disease.
Post Covid-19 Complications
Black Fungus
‘Black Fungus’ or Mucormycosis infection among COVID-19 patients could affect the sinuses, eyes, brain, lungs and can be life-threatening if left unchecked.
Who is at risk?
People who are on medication for other health problems which reduces their ability to fight environmental pathogens. A drop in immunity could be triggering these cases. High risk individuals are with diabetes or severely immunocompromised patients.
Warning signs:
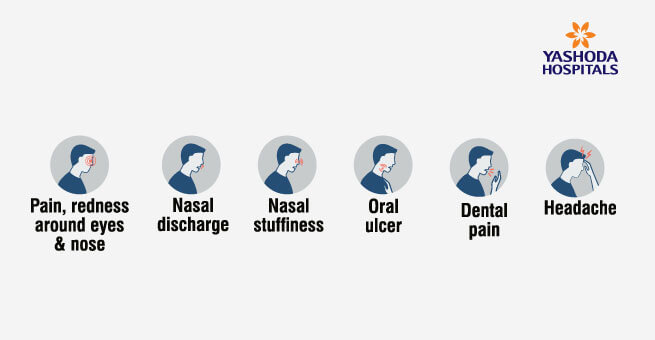
DOs
- Control hyperglycemia
- Monitor blood glucose level post COVID-19 discharge, also in diabetics
- Use steroid judiciously-correct timing, correct dose and duration
- Use clean, sterile water for humidifiers during oxygen therapy
- Use antibiotics/antifungals judiciously
DON’Ts
- Do not miss warning signs.symptoms
- Do not consider all cases with blocked nose as bacterial sinusitis
- Do not hesitate to seek aggressive investigations
- Do not lose crucial time to initiate treatment for mucormycosis
PREVENTION
- Use masks if you are visiting dusty construction sites.
- Wear shoes, long trousers, long sleeve shirts, gloves while handling soil (gardening), moss or manure.
![]()
- Maintain personal hygiene including thorough scrub baths.
![]()
Don’t ignore and Don’t panic if you see any black fungus symptoms. Consult our ENT specialists immediately
Post Covid-19 Complications
Long Covid Syndrome
Long Covid refers to when people continue to experience symptoms of Covid-19 and do not fully recover for several weeks or months after the start of their symptoms. It can happen to anyone who has had Covid-19, even if the illness was mild, or they had no symptoms. People with Long Covid report experiencing different combinations of the Covid-19 symptoms.
People can discuss a treatment plan with a doctor. Taking steps to look after their health and well-being, such as by following a healthy diet, getting plenty of rest, and doing gentle exercise may all help a person manage Long Covid.
Multisystem Inflammatory Syndrome in Children (MIS-C)
Multisystem inflammatory syndrome in children (MIS-C) is a serious condition that appears to be linked to children who become infected with the COVID-19 , in some rare cases go on to develop MIS-C that may show up weeks after COVID-19 infection.
In this condition some organs and tissues such as the heart, lungs, blood vessels, kidneys, digestive system, brain, skin or eyes become severely inflamed and without treatment, could be life-threatening.
Produces varying symptoms in children, but they can include:
- Fever
- Neck pain
- Abdominal pain
- Rash
- Vomiting
- Bloodshot eyes
- Diarrhea
- Feeling extra tired
If your child has any of the warning signs listed above, get care immediately. Take your child to the hospital

Click here to download the PDF for Post Covid Care Guidelines for People Recovering Post Covid-19 (Download PDF)















 Appointment
Appointment Call
Call More
More