Does Osteoporosis Increase the Risk of Fractures?

1. What are the types of osteoporosis?
2. What is peak bone mass, and how is it related to osteoporosis?
3. Does osteoporosis increase the risk of fractures?
4. Who is at increased risk of developing osteoporosis?
5. How do you detect osteoporosis?
6. Who should receive routine screening for osteoporosis?
7. What are the available treatment options?
Have you ever had a fracture with the slightest hint of pressure? Or have you ever seen any elderly people who had multiple fractures as a result of their weak and fragile bones? If you answered yes, you are well aware of the cause: osteoporosis, the silent disease that is the leading cause of bone fractures.
The term “osteoporosis” translates to “porous bone,” which means that the disease weakens the bones due to decreased bone mass and strength, putting you at a higher risk for unexpected bone fractures.
The disease develops without causing any symptoms, and it is usually not discovered until the weakened bones cause fractures, hence the term “silent disease.”
This article gives you a thorough understanding of osteoarthritis and walks you through the causes, types, diagnosis, and treatment options
What are the types of osteoporosis?
Osteoporosis is classified into two types, primary and secondary, based on its underlying causes.
While primary osteoporosis is caused by age-related, natural changes in bone density, secondary osteoporosis is caused by other underlying conditions or as a side effect of medications.
- Primary Osteoporosis
Type I osteoporosis, also known as postmenopausal osteoporosis, occurs after menopause due to a significant decrease in oestrogen levels, which play an important role in bone health and thus result in bone damage.
Type II osteoporosis, also known as senile osteoporosis, usually develops in people over the age of 70, as ageing causes bone tissue weakening and thus impairs the body’s ability to form new bone.
Both of the two primary types of osteoporosis are far more common in women than in men.
- Secondary Osteoporosis
Secondary osteoporosis develops as a result of certain medications and/or medical conditions, such as those affecting the endocrine system, bone marrow, gastrointestinal system, seizure disorders, eating disorders, and cancer, among others.
Because primary and secondary causes of osteoporosis frequently require different treatments, it is crucial to distinguish between them. To ascertain the cause, a complete medical history, a physical examination, and the appropriate diagnostic tests are needed.
Apart from primary and secondary types, there are two other types of osteoporosis.
- Osteogenesis Imperfecta
Osteogenesis imperfecta is a very rare form of osteoporosis that occurs as a result of a genetic mutation. It ranges in severity from mild to severe and is similar to traditional osteoporosis. However, it may also present with additional symptoms such as respiratory issues, height defects, and an abnormally small rib cage.
- Idiopathic Juvenile Osteoporosis
Idiopathic juvenile osteoporosis affects children, has no known cause, and typically manifests just before puberty. Apart from brittle and porous bones, this condition is not associated with any other symptoms and usually gets resolved without any medical treatment after a relatively short period of time.
Did you know that osteoporosis often remains undetected until a bone fracture occurs?
What is peak bone mass, and how is it related to osteoporosis?
While bone mass is a measure of the amount of bone in the body, peak bone mass (PBM) is the maximum bone mass attained by an individual, usually between 25 and 30 years of age.
The amount of “peak” or “maximum” bone mass that a person can develop during the first 30 years of life depends on genetics, dietary factors, health status, physical activity, exercise, and hormonal status. Beyond this age, every person gradually loses bone over the course of each year. However, the rate of loss in women after menopause may be higher.
According to studies, a 10% increase in PBM reduces the risk of osteoporosis-related fractures in older adults by 50%, making it critical in determining the risk of osteoporotic fractures. As a result, achieving a high PBM during the first three decades of life would significantly contribute to osteoporosis prevention.
Does osteoporosis increase the risk of fractures?

Yes. In fact, osteoporosis is the leading cause of fractures in people over the age of 60. Osteoporosis makes the bones weak and brittle, making them more prone to fractures from minor falls and injuries, many of which go unnoticed and are only detected during screening.
Approximately 90 lakh osteoporotic fractures occur worldwide each year, according to studies, with the number likely to be higher because many fractures go undetected. These figures are expected to rise even more in the coming years, eventually reaching epidemic proportions in the coming decades.
Who is at increased risk of developing osteoporosis?
Men and women of all races are susceptible to osteoporosis. However, lifestyle habits, medications, and underlying comorbidities all have an impact on the disease’s risk. The following are the most frequently observed risk factors.
- Age
- Gender (Women)
- Menopausal women
- Poor nutrition
- Low vitamin D and calcium
- Sedentary lifestyle
- Alcoholism
- Smoking
Additionally, long-term use of certain medications, such as proton-pump inhibitors, corticosteroids, aspirin, anxiolytics, sedatives, antidepressants, chemotherapy, and radiation therapy, increases the risk of osteoporosis.
While osteoporosis has an impact on all bones, some parts of the body, such as the wrists (distal forearm), hips (proximal femur), and spine (vertebrae), have a higher propensity to fracture.
How do you detect osteoporosis?
Your bone health can be determined with the help of a bone mineral density (BMD) test. A central dual-energy x-ray absorptiometry, or central DXA test, is the BMD test that is most frequently performed. It helps with osteoporosis detection, determines your risk for fractures, and evaluates how well you respond to osteoporosis treatment. It is painless and comparable to having an x-ray.
It calculates your score by measuring your bone mineral density and comparing it to a predetermined standard.
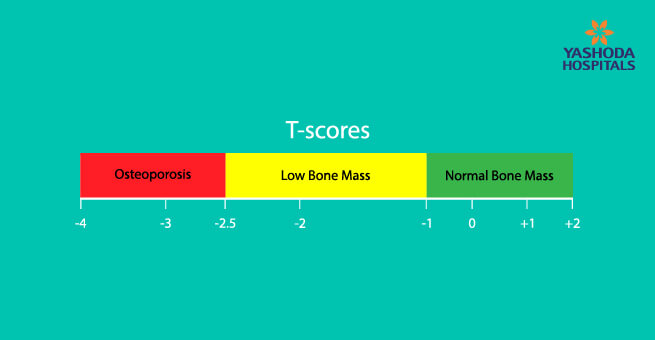
T-Score:
The T-score, which is expressed in units called standard deviations (SDs), is calculated by comparing the BMD test results to the bone mineral density of a healthy young adult (an average 30-year-old). A score of 0 indicates that your BMD is within the normal range for a healthy young adult.
The more standard deviations below zero, indicated by negative numbers, the lower your BMD and the greater your risk of fracture.
Normal: +1 or −1 SD
Low bone mass: −1 to −2.5 SD
Osteoporosis: −2.5 SD or lower
Z-score:
A Z-score compares a person’s BMD to the average BMD of people of the same age and gender. It is used to diagnose secondary osteoporosis in children, young adults, premenopausal women, and men under the age of 50.
Your bone density is only one of many factors that influence your bone health. Other factors include your family history, medical conditions, and medications.
Who should receive routine screening for osteoporosis?
The National Osteoporosis Foundation (NOF) recommends measuring BMD for the following individuals:
- Women above 65 years and men above 70 years of age, regardless of risk factors.
- Postmenopausal women below 65 years and men between 50 to 69 years of age with risk factors for fracture.
- High-risk individuals: Adults with rheumatoid arthritis or taking medications (long-term steroid therapy), diabetics, and women attaining early menopause, among others.
What are the available treatment options?
The course of treatment is determined by the underlying cause, the severity, and the risk of future fracture (as determined by various scoring systems like the FRAX tool). The first step is to address modifiable factors such as diet, nutrition, vitamin D, and quitting smoking and drinking.
There are two broad categories of drugs available:
Antiresorptive agents
Anti-resorptive agents work by slowing the rate of bone loss. They consist of bisphosphonates (alendronate, risedronate, ibandronate, and zoledronic acid), denosumab, calcitonin, and raloxifene.
Anabolic agents
Anabolic agents work by stimulating bone formation. They consist of teriparatide and abaloparatide.
They can be administered weekly, once every two weeks, or once every six months, and come in a variety of formulations, including oral tablets and injections.
The typical course of therapy lasts between 12 and 24 months, after which, depending on the outcome, a different medication is recommended.
How does exercise aid in the prevention of osteoporosis?
Throughout life, the body continuously creates new bone and removes old bone. Osteoporosis develops when this equilibrium shifts in favour of bone resorption.
New bone is formed in response to physical stress caused by increased muscle activity, and the simplest way to achieve this is through regular exercise, which includes weight-bearing activities such as walking, jogging, and fast walking, as well as resistance training (lifting weights and resistance band exercises).
It is recommended to exercise for 120 to 300 minutes per day, or four days per week on average. The frequency, duration, and intensity of the exercise may vary.
What are the precautionary measures?

If you are diagnosed with osteoporosis, in addition to taking medication, the following habits are essential for managing the condition.
- Exercise
Exercises that strengthen bones and lower the risk of fracture. The more active and fit you are as you get older, the less likely it is that you will fall and break a bone.
- Nutrition
Eat a healthy diet, and make sure you get enough calcium and vitamin D.
- Quitting smoking
Cigarette smoking accelerates bone loss.
- Limiting alcohol intake
Moderation is key if you decide to consume alcohol. Do not exceed the recommended number of drinks per day.
Osteoporosis increases the likelihood of bone fractures. However, there are numerous steps that people with osteoporosis can take to reduce their fracture risk and live a healthy life. Aside from taking steps to strengthen bones and prevent falls, there are medications that can be used to treat osteoporosis.
References:
- Osteoporosis
https://www.mayoclinic.org/diseases-conditions/osteoporosis - Types and Causes of Osteoporosis
https://www.spine-health.com/conditions/osteoporosis - What Causes Postmenopausal and Senile Osteoporosis?
https://www.spine-health.com/conditions/osteoporosis - Types of Osteoporosis
https://www.parisorthopedic.com/types-of-osteoporosis - The importance and relevance of peak bone mass in the prevalence of osteoporosis
https://pubmed.ncbi.nlm.nih.gov - Bone health 2022: an update
https://www.tandfonline.com - How Likely Is It That I Will Break a Bone If I Have Osteoporosis?
https://www.healthline.com/health/managing-osteoporosis - Bone Mass Measurement: What the Numbers Mean
https://www.bones.nih.gov/health-info/bone/bone-health/bone-mass-measure - Understanding Bone Density Results
https://americanbonehealth.org/bone-density - Osteoporosis screening recommendations
https://www.uptodate.com/contents
About Author –
Dr. Praveen Kumar, Consultant Orthopedic & Joint Replacement Surgeon, Yashoda Hospitals – Hyderabad
MS (Ortho), Fellow Joint Replacement

















 Appointment
Appointment Call
Call More
More