Deep Vein Thrombosis (DVT)
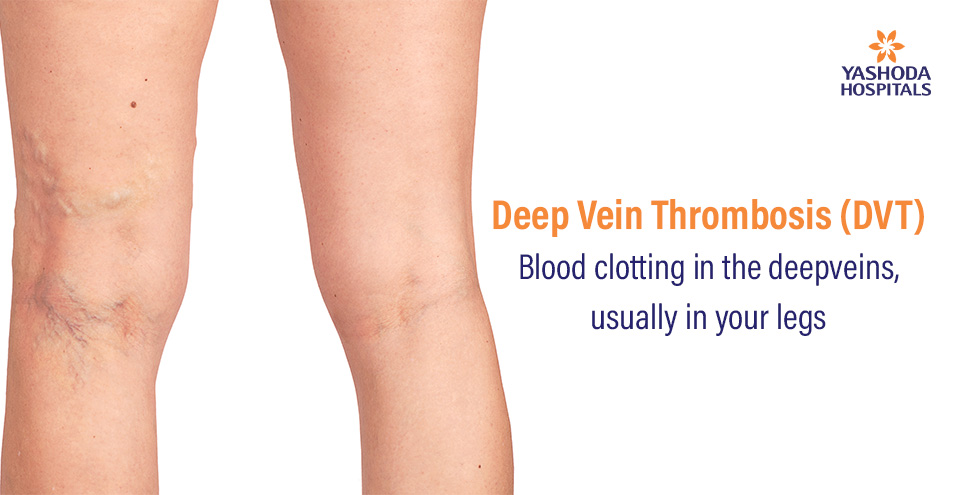
Deep vein thrombosis (DVT) occurs when a blood clot (thrombus) forms in one or more of the deep veins in your body, usually in your legs. Deep vein thrombosis can develop if you have certain medical conditions that affect how your blood clots. It can also happen if you don’t move for a long time, such as after surgery or an accident, or when you’re confined to bed.
Symptoms
- Swelling: Swelling in your foot, ankle, or leg, usually on one side.
- Pain: Cramping pain in your affected leg that usually begins in your calf.
- Warmth to the touch: An area of skin that feels warmer than the skin on the surrounding areas.
- Redness of the leg or arm: Skin over the affected area turning pale or a reddish or bluish color
Risk Factors
- Prolonged sitting or immobility
- Recent Surgery
- Recent trauma to the lower body
- Obesity
- Pregnancy or recent childbirth
- Heart Attack or Heart Failure
- Rare genetic conditions that affect blood clotting factors
Treatment
Treatment is focused on clearing the clot and preventing pulmonary embolism. They include:
- Thrombolysis followed with blood thinners
- Thrombus aspiration
Preventions
- If you have had surgery or have been on bed rest for other reasons, try to get moving as soon as possible. If you’re sitting for a while, don’t cross your legs, which can hamper blood flow.
- Lose weight and quit smoking
- Regular exercise lowers your risk of blood clots, which is especially important for people who sit a lot or travel frequently.
- Blood Thinners don’t break up existing blood clots, but they can prevent clots from getting bigger and reduce your risk of developing more clots
- Compressions Stocking pressure helps reduce the chances that your blood will pool and clot.
- If you can’t take medicines to thin your blood, you might have a filter inserted into a large vein – the vena cava – in your abdomen. A vena cava filter prevents clots that break loose from lodging in your lungs.
MYTH: I am really active and in grate shape , so dont need to worry about getting DTV
FACT: Almost anyone can be affectedby DTV: younger or old , couch potato to athlete. Athletes are at incresed risk if they’ve experenced recent physical injury, are dehyderate ,and/ or partake in long distance travel for games and other events
MYTH: I ve never even heard of DVT it cant be that serious.
FACT: Deep-vein thrombosis (DVT) is a serious and under diagnosed medical condition that result when a blood clot forms in a vein.
About Author –
Dr. Bhavin L. Ram, Consultant Vascular & Endovascular Surgery, Yashoda Hospital, Hyderabad.
MS, DNB (Vascular Surgery)














 Appointment
Appointment Call
Call More
More