Brain stroke and treatments
1. What is a stroke or brain attack?
2. What are the signs and symptoms of a stroke?
3. What are the types of stroke?
4. What are the risk factors of stroke?
5. How do doctors diagnose a stroke?
6. What are the treatments for brain stroke?
7. What are the complications of stroke?
8. What can a person expect during rehabilitation and recovery after a stroke?
What is a stroke or brain attack?
A stroke is a medical condition that occurs due to the blockade or rupture i.e bursting of a blood vessel carrying oxygen and nutrients to the brain. Disruption of the blood supply and consequently oxygen to a part of the brain can lead to cell death of that part. Prompt treatment of stroke is extremely crucial to prevent any long term or permanent damage, making stroke a medical emergency.
What are the signs and symptoms of a stroke?
Some of the most commonly reported signs and symptoms of stroke include:
- Difficulty in speaking and comprehension: There may be associated confusion, slurring of speech, and difficulty in understanding someone else’s speech.
- Paralysis or numbness: A person may experience sudden numbness, weakness, or paralysis in parts of the body, mostly on one side like the face, arm, or leg.
- Difficulties of vision: A person may experience any of the following disturbances of vision namely double, blurred, or blackening either in one or both eyes.
- Sudden, severe headache: The headache associated with a stroke may be sudden, severe, and associated with vomiting, dizziness, or loss of consciousness.
- Difficulty walking: A person may experience sudden dizziness or a loss of coordination and loss of balance.
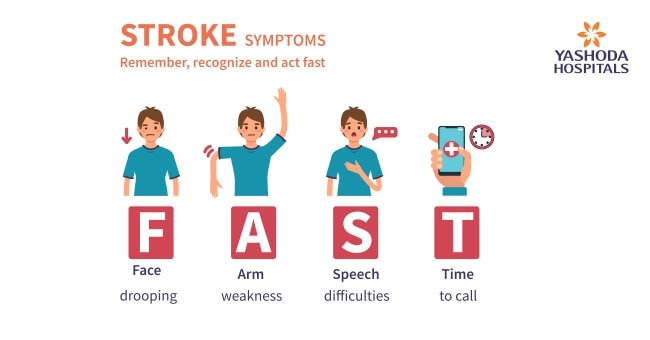
Medical attention should be sought immediately if a person notices someone having any signs or symptoms of a stroke. Even though they sometimes may come and go or completely disappear, medical attention should be sought immediately. If a stroke is suspected, a quick regime called FAST can be attempted to verify it:
- Face: The person should be asked to try smiling. If one corner of the mouth droops to a side on smiling, a stroke should be suspected.
- Arms: The person should be asked to raise both the arms together over the head. A stroke should be suspected if the person is unable to raise an arm or if one arm begins to fall to one side or drifts downward.
- Speech: The person should be asked to repeat simple words or phrases. Slurring of speech or deviation from the way of speaking should raise a suspicion of stroke
- Time: If any of these signs are observed, time is of utmost importance. Emergency medical help should be sought immediately. Particular attention to the time when symptoms begin to appear should be given. This is crucial because the effectiveness of some treatment options depends on the lapse between the appearance of symptoms and the time of intervention.
What are the types of stroke?
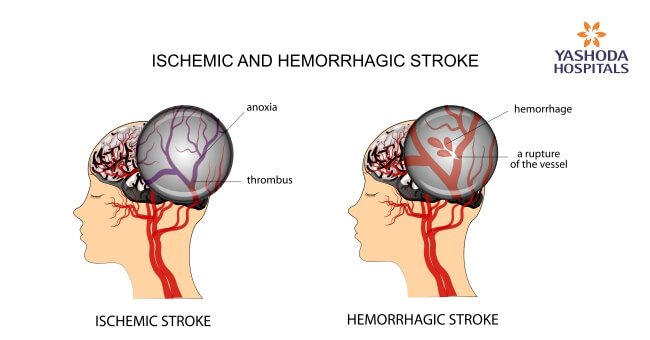
A stroke is primarily of two types, namely ischemic or hemorrhagic stroke. Sometimes a person may have a disruption of blood flow to the brain that lasts temporarily and doesn’t lead to lasting symptoms. The condition is known as a transient ischemic attack (TIA).
Ischemic stroke
This is the most common type of stroke that occurs due to a blockage in an artery. Narrowing or blocking the brain’s blood vessels may lead to a severely reduced blood flow or ischemia to the parts of the brain supplied by the vessel. Conditions like atherosclerosis i.e building up of fatty deposits within the blood vessels or formation of blood clots locally or those travelling through the bloodstream can block the blood vessels to cause an ischemic stroke.
Hemorrhagic stroke
Type of stroke that occurs due to leakage from within or bursting of a blood vessel. Brain haemorrhages can result from many conditions that affect the blood vessels. Depending on the location of the haemorrhage, the stroke is of two types namely:
- Intracerebral haemorrhage (ICH): Occurs within the brain tissues or ventricles
- Subarachnoid haemorrhage (SAH): Occurs within the space between the brain and the tissue covering the brain
Arteriovenous malformation: Rupturing of an abnormal tangle of thin-walled blood vessels can sometimes lead to a less common cause of bleeding in the brain.
Transient ischemic attack (TIA)
Sometimes, ischemia or decrease in blood supply to the brain may last very briefly, as little as five minutes and it doesn’t cause permanent damage. The condition is known as TIA or mini-stroke. A TIA like an ischemic stroke may be caused due to blockage due to a clot or debris that temporarily reduces the blood flow to a part of the nervous system and then resolves.
However, it is not always possible to differentiate between a stroke or TIA based on a person’s symptoms. So emergency care should be sought even if a TIA is suspected. TIA may occur due to a partially blocked or narrowed artery to the brain that increases a person’s risk of having a full-fledged stroke later.
What are the risk factors of stroke?
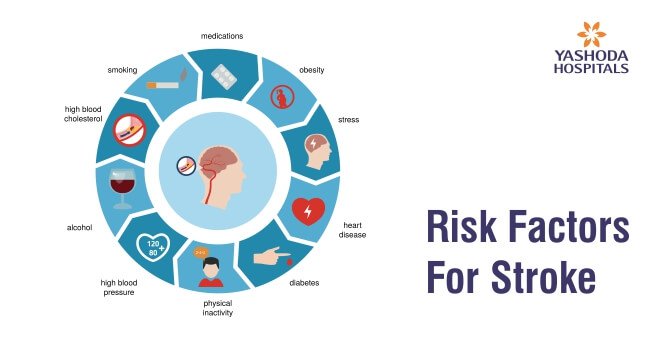
The risk of stroke increases due to many factors, some of which are as follows:
- Age: Persons of age over 55 years are usually at a higher risk of stroke than younger people.
- Sex: The risk of stroke is usually higher in men than in women. Strokes are more common in older women and the mortality, i.e the likelihood of dying due to a stroke is higher in women than men.
- Hormones: Hormone therapies containing estrogen or the use of contraceptive pills can increase the risk of stroke.
Lifestyle-related risk factors
- Obesity or excess weight
- Sedentary lifestyle
- Alcohol and substance abuse with agents such as smoking tobacco or drugs like cocaine and methamphetamine
Risk factors associated with medical conditions
- Hypertension or high blood pressure
- Hypercholesterolemia or high cholesterol
- Diabetes
- Disorders of sleep like obstructive sleep apnea
- Cardiovascular diseases like heart defects, infections within the heart or abnormalities of heart rhythm such as atrial fibrillation, heart failure
- Presence of a personal or family history of stroke, TIA or heart attack
- Prolonged use of anticoagulants or blood thinners
- Anatomical defects like aneurysms i.e bulge at weak spots in the blood vessel walls
- Accidental injuries to the head i.e trauma such as a road traffic accident
How do doctors diagnose a stroke?
Since stroke is an emergency condition, the diagnosis of stroke should be done swiftly and the medical emergency team at the hospital tries to determine what type of stroke is the person having. Imaging tests are carried out soon after arrival at the hospital.
Diagnosis is usually made based on the below parameters:
History and physical examination: After taking a quick medical history, a physician does a quick physical examination to assess a person’s physical and neurological state.
Blood tests: Several blood tests to check parameters like clotting time, blood sugar, infection, etc. are ordered.
Imaging tests:
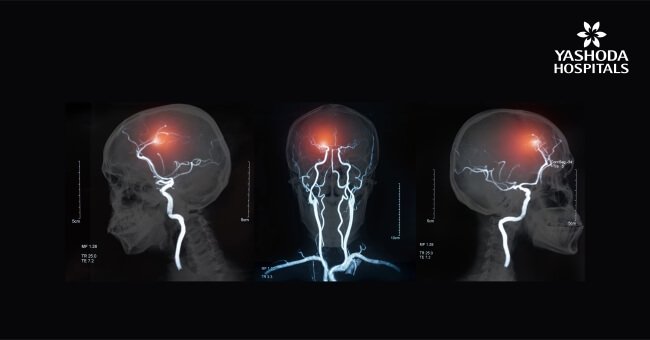
- Computerized tomography (CT) scan is done to visualize the exact place of bleeding in the brain and the possible cause like an ischemic stroke or presence of a tumour or other conditions. To view the blood vessels in the neck and brain in greater detail, a dye may be injected and the procedure is called computerized tomography angiography.
- Magnetic resonance imaging (MRI): An MRI may be done to identify tissues damaged by an ischemic stroke and brain haemorrhages. To view the arteries and veins distinctly and highlight the blood flow, doctors may need to inject a dye in a procedure known as magnetic resonance angiography or magnetic resonance venography.
- Carotid ultrasound: Presence of fatty deposits and blood flow in the carotid arteries which are the main arteries of the brain and neck can be done using this procedure
- Echocardiogram: The procedure is done to determine any source of clots in the heart that may have travelled to the brain and leading to a stroke.
What are the treatments for brain stroke?
The emergency treatment for stroke is dependent on the type of stroke a person has, i.e an ischemic stroke or a hemorrhagic stroke.
Ischemic stroke
The goal of treatment after an acute ischemic stroke is the restoration of blood flow to the affected area of the brain as soon as possible, ie, within the first few hours after the onset of the symptoms of stroke symptoms. Speed of treatment is a critical factor in determining treatment outcomes for persons with disabling acute ischemic stroke (AIS). AIS can progress rapidly and lead to potential long term effects if not treated in time.
The main treatments for ischemic stroke are:
Thrombolytic therapy: A medication called alteplase or “tPA” is administered through a vein (IV) to break up the clot that may be blocking blood flow to the brain. The therapy should preferably be given within 4.5 hours from the onset of symptoms when given intravenously. A quick treatment with tPA not only improves the survival chances of a person but also may reduce complications. tPA dissolves the blood clot to restore the blood flow. Your doctor will consider certain risks, such as potential bleeding in the brain to determine if tPA is appropriate for you.
Sometimes tPA may be directly delivered into the brain by inserting a catheter i.e a long, thin tube through an artery in the groin which is gradually advanced to the brain to deliver tPA directly at the site of the stroke. The time window for this treatment is limited too, but is somewhat longer than for injected tPA, but is still limited.
Mechanical thrombectomy: In this procedure, a specialist places a catheter with a “stent retriever device” or suction in the blocked blood vessels and the clots are directly removed from the brain.
For persons with large clots that can’t be completely removed with tPA, mechanical thrombectomy is beneficial. It is usually performed in combination with injected tPA.
With the advent of newer imaging technologies, the time window when these procedures can be considered has been gradually increasing. Perfusion imaging tests CT or MRI techniques can help the doctors in determining how likely is a person to benefit from procedures like mechanical thrombectomy.
Other procedures
Sometimes, to decrease a person’s risk for another stroke a procedure to open up an artery that’s narrowed by plaque may be advised. Some of the options include:
- Carotid endarterectomy: Removal of plaque that is potentially blocking a carotid artery can reduce the risk of ischemic stroke.
- Angioplasty and stents:Angioplasty and placement of stents in the major arteries of the heart that are blocked with plaque can help in reducing the risk of a stroke.
Hemorrhagic stroke: The main objective of emergency management of hemorrhagic stroke is to control the bleeding and reduce pressure on the brain that may be caused due to the formation of a blood clot or excess fluid accumulation. The treatment options for hemorrhagic stroke include:
Medication: If the scan shows a hemorrhagic stroke, a doctor may take the following therapeutic approach:
- Administer medicines to reduce potential damage to brain damage due to bleeding
- Administer medicines to reduce blood pressure if it is too high
- If a person is on blood-thinning medicines, some alternative medicines may be administered to help the blood clot to stop bleeding. Any medicines that a person is taking for thinning the blood or prevent it from clotting should be stopped.
Surgery: Depending on the severity of the symptoms and associated factors, some persons may require surgery. Doctors do surgery to either remove a collection of blood if it is pressing down on the brain or causing the brain to swell or to stop the bleeding in the brain and fix the damaged blood vessel that was bleeding.
Surgery may usually be done within the first 48 to 72 hours after the haemorrhage. If the affected person is not in a stable condition, the surgery may be delayed until one to two weeks. Some of the surgical options are:
- Aneurysm treatment: An aneurysm is a weakened area in a blood vessel that balloons out. Rupturing of the blood vessel may lead to bleeding causing a hemorrhagic stroke.Since the risk of a subarachnoid hemorrhage and brain damage is quite high in the case of aneurysm rupture, emergency surgery may be required. Types of surgical intervention are:
- Surgical clipping: An aneurysm is closed off with this surgical procedure. A part of the skull is removed by craniotomy to access the aneurysm and locate the feeding blood vessel of the aneurysm. A metal clip is placed on the neck of the aneurysm to obliterate the flow of the blood.
- Endovascular therapy or coiling: This is a minimally invasive procedure, less invasive than surgical clipping. The affected blood vessel is accessed with a catheter or a hollow tube that is inserted through a small incision in the groin. A guidewire is then passed through the catheter to push a soft platinum wire into the aneurysm. The blood flow to the aneurysm is cut off by coiling the wire around the base where the artery supplies blood to the aneurysm.
- Flow diverters: These are newer treatment options for a brain aneurysm, especially the larger ones which are not amenable to other forms of treatment. Flow diverters are tubular stent-like implants that act by diverting the blood flow away from the sac of an aneurysm. Once the blood movement within the aneurysm stops, the body is stimulated to heal the site and reconstruction of the parent artery is encouraged.
- Arteriovenous malformation treatment: Arteriovenous malformation (AVM) is an abnormal tangling of blood vessels connecting arteries and veins within the brain. AVMs have a significant risk of further bleeding in case of a stroke. Management options include surgery, shrinking of blood vessels with radiation or radiosurgery, or embolization techniques.
- Decompressive craniotomy: In case of a life-threatening situation due to the pressure effects of a blood clot in the brain, the neurosurgeon may consider a procedure to open the skull and/or remove the blood. Factors affecting the decision of decompression craniotomy include the location and size of the haemorrhage, the patient’s age and medical condition, and the likelihood of making a recovery from stroke.
What are the complications of stroke?
A person can experience temporary or permanent disabilities after a stroke based on how long the brain’s blood flow was obstructed and which part was affected. Complications may include:
- Problems of speech: Persons with stroke may sometimes not able to speak anymore or understand speech. This condition is known as “aphasia.” In some people the speech might become slurred, a condition known as “dysarthria.”
- Weakness and movement problems: People who have a stroke sometimes have muscle weakness or paralysis of one side of the body. The muscle weakness can affect the face, arm, and leg, a condition known as “hemiparesis.”
- Problems of walking and balancing: After a stroke, some people may have trouble walking, grasping objects, or balancing. They may not be able to make controlled, planned movements, even if the stroke did not cause weakness or loss of sensation. A condition is known as “apraxia”.
- Partial loss of sensation: After a stroke, some people may have partial or total loss of feeling on the left or right half of their body.
- Difficulty eating or swallowing: People with a stroke may sometimes have trouble swallowing or “dysphagia”. People with dysphagia may sometimes get food lodged in their windpipe or lungs which is a dangerous condition.
- Depression: Recovery can become difficult as persons with stroke tend to become depressed many times. Treatment for depression after a stroke is generally recommended.
- Problems with bladder control: Difficulty in controlling the bladder may lead to a condition known as “urinary incontinence” which causes leakage of urine. It often gets better over time.
What can a person expect during rehabilitation and recovery after a stroke?
Post-stroke care usually focuses on helping a person recover as much physical and physiological function as possible and return to independent living. The impact of stroke on a person’s physical abilities is dependent on the area of the brain that was involved and the amount of tissue damaged.
A stroke of the right side of the brain may affect the movement and sensation on the left side of the body and vice versa. Damage to the left side of the brain may also lead to speech and language disorders.
During the recovery process, the treating physician or neurologist would recommend the most appropriate therapy based on the person’s age, overall health, and extent of disability due to the stroke. The rehabilitation plan would take into consideration the person’s lifestyle, interests, and priorities, and the availability of family members or other caregivers.
Rehabilitation usually begins before the person leaves the hospital. After discharge, rehabilitation should be continued at home and follow up visits in the same hospital if possible.
Recovery needs may vary as per a person’s condition and a person may be assisted by a:
- Neurologist
- Dietitian
- Physical therapist
- Occupational therapist
- Speech therapist
- Psychologist or psychiatrist
- Occupational therapist
Conclusion
Since many of the risk factors of a stroke are controllable, adhering to the medical recommendations of the physician and some hard but required lifestyle changes can help a person in lowering the chances of having a stroke or another if he/she already has had one. Similarly, a transient ischemic attack or “TIA,” maybe a warning sign and these same things can help a person to prevent a full-blown stroke.
Medicines and lifestyle changes work simultaneously to give the most benefit. A person must take all the medicines as the doctor prescribes and also make the lifestyle changes recommended by the doctor to reduce the risk of a new stroke.
References:
- Mayo Clinic. Brain Aneurysm. Available at: org/diseases-conditions/brain-aneurysm/symptoms-causes/syc-20361483. Accessed on April 21, 2020
- Mayo Clinic. Stroke. Available at: https://www.mayoclinic.org/diseases-conditions/stroke/symptoms-causes/syc-20350113. Accessed on April 21, 2020
- Stroke. Available at: https://www.cdc.gov/stroke/index.htm Accessed on April 21, 2020
- Medline Plus. Stroke. Available at https://medlineplus.gov/stroke.html. Accessed on April 21, 2020


















 Appointment
Appointment Call
Call More
More