Bariatric Surgery Treatment in Hyderabad, India
According to World Health Organization (WHO), being obese or overweight is no more just a cosmetic issue, rather a chronic health issue that affects person’s overall wellbeing and increases risk to other chronic diseases.
Obesity Treatment in Hospital Hyderabad
What is obesity?
Obesity is a health condition noted with an excessive accumulation of body fat. By and large, obesity can be accessed in terms of height, body build, and adiposity index or BMI index. It is defined by a quantifiable measure, body mass index (BMI). Anyone with a BMI of more than 25 Kg/square metre is considered overweight and more than 30 is considered obese.
Obesity is progressive in nature. Early-onset obesity in children has long-lasting implications on their growth and health as an adult. It is important to identify the condition and the causative factors early. Obesity may be caused due to sedentary lifestyle or medical causes such as underactive thyroid (hypothyroidism), Cushing’s syndrome etc.
Morbid obesity is a serious condition wherein the excess body weight cannot be successfully dropped easily and poses greater health threats such as diabetes, high blood pressure, sleep apnea, gastroesophageal reflux disease (GERD), gallstones, osteoarthritis, heart disease, and cancer. Morbid obesity is defined by a BMI of 35 or more with any of the above obesity-related health condition or by a BMI of 40 or more.
What is body mass index?
Doctors use body mass index as a measure of excess body weight and define the grade of obesity. Body mass index is the ratio of weight (in kgs) to height in meters squared.
| Category | BMI Range |
|---|---|
| Normal Size | 18.9 to 24.9 |
| Overweight | 25 to 29.9 |
| Class I, Obesity | 30 to 34.9 |
| Class II, Serious Obesity | 35 to 39.9 |
| Class III, Severe Obesity | 40 and greater |
Weight Loss Treatment in Hyderabad
Bariatric surgeries:
Bariatric surgery is the weight loss option for morbid obese patients who are at increased risk or are diagnosed with major health conditions such as diabetes, joint disorders, hypertension, high cholesterol, sleep apnea etc. Doctors recommend bariatric surgery for those who are morbidly obese and have tried and failed to lose weight by conservative approaches.
Laparoscopic Adjustable Gastric Banding (LAGB):
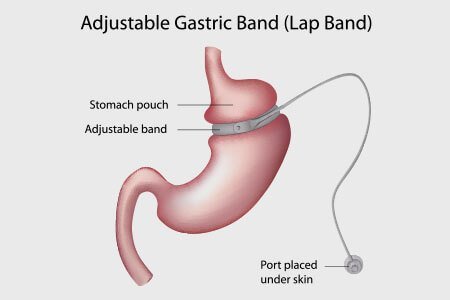
During laparoscopic adjustable gastric banding surgery, an inflatable band is placed around the upper stomach that restricts the space to hold ingested food. The band is placed in such a way that the upper stomach forms a small pouch which is separated from the remaining portion of the stomach with a narrow opening, maintained by the inflation of the band. The band is then connected to a port that is placed under the skin of the abdomen.
After surgery, thickness of the band is adjusted to adequately obstruct flow of food and delay gastric emptying. By injecting or removing fluid through the port, the thickness of the band is adjusted and in turn the opening is suitably restricted/expanded.
Thus, gastric banding is a restrictive weight loss surgery which improves saitety and weight loss. However, it does not affect the person’s ability to absorb calories and nutrients.
Laparoscopic Gastric Sleeve Resection (LGSR):
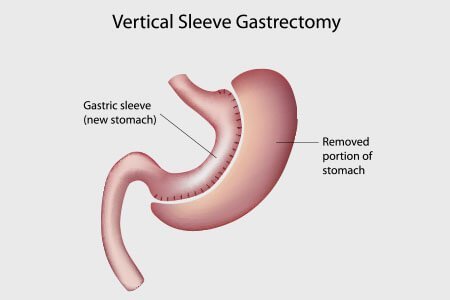
In Laparoscopic gastric sleeve resection, a major portion of stomach is removed along the major curve of the stomach and the remaining stomach is formed into a tube-like structure. The procedure permanently reduces the size of the stomach. Similar to laparoscopic adjustable gastric banding surgery, it is a restrictive weight loss surgery which improves satiety and weight loss. it also reduces the appetite due to lesser appetite-regulating hormone, ghrelin. However, it does not affect the person’s ability to absorb calories and nutrients.
Roux-en-y Gastric Bypass (RYGB):
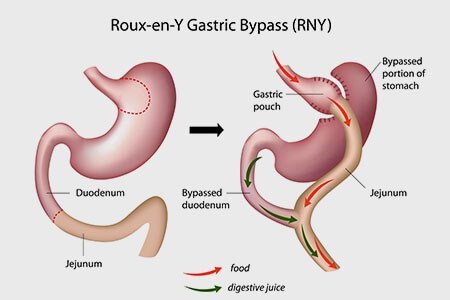
In gastric bypass the stomach is divided into a small upper pouch and a much larger, lower pouch. The upper small pouch is then connected to the small intestine, so the ingested food bypasses the remaining lower portion and duodenum. The connection between lower pouch and the duodenum with the small intestine is retained intact, so the digestive juices reach the small intestine and aid in digestion.
In contrast to laparoscopic gastric sleeve resection, the rest of the stomach is left in place and continues to remain healthy. This reduces the amount of food taken and thus the calories consumed. Bypassing part of the intestine also results in fewer calories being absorbed.
Biliopancreatic diversion with duodenal switch:
A major portion of stomach is removed as in gastric sleeve surgery and the remaining pouch is directly connects to the final segment of the small intestine. This way the food passes through the small portion of the stomach and passes directly into the final segment of small intestine and into the colon. However, before the food enters colon, it gets mixed with the bile and the pancreatic juices in the small intestine.
Deodenal switch: The duodenum along with the valve is then connected to the last part of the small intestine directly. This portion remains healthy and receives bile and pancreatic juices through the biliopancreatic diversion.
FAQ’s
Are there any long-term side effects or health considerations after the surgery?
Nerve damage, muscle weakness, breathing damage, lymphedema and postoperative cognitive dysfunction (POCD), are a few long-term side effects after a bariatric surgery.
What is the recovery time and process after bariatric surgery?
The recovery phase depends on the complexity of the surgery, and the surgeon’s expertise and experience. However, there are some common points to consider after the procedure like hospital stays 1-3 days after surgery and having only a liquid diet initially after 1-2 days of not eating anything.
How much weight can I expect to lose after bariatric surgery?
Based on the type of surgery performed be it gastric banding, gastric bypass, or sleeve gastrectomy a patient is expected to lose 40% to 70% of their body weight.
What are the potential risks and complications associated with bariatric surgery?
Bariatric surgery has potential complications that can occur immediately after or months later, including gallstones, hair loss, loose skin, acid reflux, dilation of the oesophagus, obstruction of the stomach, gastric leak, nausea and vomiting.
What are the different types of bariatric surgery, and how do they differ?
There are four main types of bariatric surgery namely gastric bypass, adjustable gastric, sleeve gastrectomy, and biliopancreatic diversion with duodenal switch.



 Appointment
Appointment Call
Call More
More