Uterine Fibroids: Symptoms, Causes, Diagnosis & Treatment Options

Not Just Cramps: Reality Of Uterine Fibroids
Uterine fibroids start as a silent discomfort, something easy to ignore, something a woman tells herself in the beginning: “This too shall pass.” But slowly, it hangs around, grows, and starts to meddle with her energy, her comfort, and her sense of normalcy. Her own body feels heavier, tired, and unpredictable. Normal days can begin to feel physically and emotionally draining. Uterine fibroids are a condition that can delicately yet deeply affect a woman’s overall well-being, mostly without clarity or answers. Yet, a woman needs to hold on to one truth that is not the end of control over your body.
Uterine fibroids are non-cancerous growths that emerge from the muscular layer of the uterus. These fibroids are very common and are often seen in women during their reproductive years. Even though fibroids are benign and do not spread like cancer, they can still cause substantial symptoms. Fibroids can be of different sizes and numbers; some are very small, while others can grow large enough to cause visible distension of the abdomen (inflated balloon-like feeling). It is very much possible for a woman to have multiple fibroids at the same time, each differing in size as well as location.
The growth of uterine fibroids is affected by hormones like estrogen and progesterone, hence they are most commonly observed during the reproductive years. Nevertheless, fibroids can also be identified after menopause, mainly if they had developed before, or due to hormonal factors. Even though they mostly decrease after menopause, they might not disappear completely. Realizing this assists in identifying signs of uterine fibroids and, therefore, the pursuit of timely care at any stage of life.
The Location Is What Changes Everything: Types Of Fibroids
The uterine fibroids are sorted according to where they are located within the uterus, and sorting fibroids is absolutely vital because it affects both symptoms and their treatment options.
| Type Of Fibroid | Location In The Uterus | Description | Common Symptoms |
| Intramural Fibroid | Within the muscular wall | As the location suggests, this type of fibroid grows inside the muscle layer of the uterus. | Heavy bleeding and a mass in the abdomen, and pressure symptoms like urinary retention and incomplete voiding. |
| Submucosal Fibroid | Inside the uterine cavity | This fibroid type grows just below the inner lining of the uterus. | Heavy bleeding and fertility issues. |
| Subserosal Fibroid | On the outer surface | This fibroid type grows outward into the abdominal cavity. | Pressure on the bladder or bowel, constipation, and Red degeneration. |
| Pedunculated Fibroid | Attached by a stalk | This type is connected to the uterus by a thin stalk. | Sudden pain on the twist of the stalk. |
The Beginning That No One Notices: How Uterine Fibroids Take Shape
What precisely leads to the development of uterine fibroids is not completely understood, but research has shown that several factors contribute to the development of uterine fibroids.
The most vital cause is the influence of hormones estrogen and progesterone, which play a major role in stimulating the growth of uterine fibroids. These hormones cause the cells inside the uterine muscles to multiply more quickly than usual.
Another factor apart from hormones that can cause uterine fibroids is genetic factors. Some women acquire a tendency to develop fibroids, mainly if there is a family history of the uterine fibroids condition. Additionally, some growth factors in the body support the formation of fibrous tissue, which helps in the development of uterine fibroids.
Uterine fibroids produce and respond to biological messengers called growth factors. Substances like Insulin-like growth factor act locally to promote the development of tumors.
The bulk of the fibroid size is not mostly from the muscle cells themselves, but from the extracellular matrix (ECM), a structural frame that surrounds the muscle cells.
Why Uterine Fibroids Happen To Some And Not Others: The Risk Of Uterine Fibroids
Understanding the risk factors of uterine fibroids assists doctors and patients in gaining early awareness, prevention wherever possible, and getting timely medical care.
Age:
Age is one of the most substantial risk factors for uterine fibrosis. Uterine fibroids are rarely seen before puberty and are most commonly identified between the ages of 30 and 50 years. As a woman ages, her body gets exposed to estrogen and progesterone for a long time. This lengthy hormonal exposure increases the chances of abnormal growth of uterine muscle cells. Over time, repeated menstrual cycles and hormonal stimulation contribute to the development of uterine fibrosis.
Although uterine fibroids mostly decrease in size after menopause due to reduced hormone levels, fibroids might still be present and identified later in life.
Hypertension (High Blood Pressure):
Hypertension is progressively identified as a vital risk factor for uterine fibroids. Hypertension and uterine fibroids have a two-way relationship where high blood pressure contributes to uterine fibroid formation; similarly, uterine fibroids might also worsen or be associated with hypertension.
High blood pressure affects the blood vessels all over the body, including those supplying blood to the uterus. Due to hypertension, when the blood vessels are exposed to continuous pressure, they are damaged, the body attempts to repair the damage, and the process might therefore involve the growth of smooth muscle cells, since fibroids are made of smooth muscle tissue.
Also, hypertension is related to increased inflammation and the release of growth-promoting substances, which further encourage uterine fibroid development.
Vitamin D Deficiency:
Vitamin D plays an important role in managing cell growth and preventing unusual cell proliferation. When the levels of vitamin D are low, the body loses some of its capacity to control the extravagant growth of uterine muscle cells. This might allow fibroids to develop or grow more quickly.
Hormonal Factors:
Uterine fibroids are highly sensitive to hormones, mainly estrogen and progesterone. These hormones stimulate the growth of uterine tissue and fibroids. These are the reasons why uterine fibroids are most often observed in reproductive years, and might grow during pregnancy when the levels of hormones are high.
Family History:
Genetics plays a substantial role in the development of fibroids. Women with a family history of uterine fibroids are increasingly likely to develop them. Especially if the mother or sister has fibrosis, the risk of fibrosis is higher due to shared genetic traits.
Obesity and Increased Body Weight:
Fat tissue produces estrogen, which can increase the growth of uterine fibroids, and obesity is also related to inflammation and metabolic changes, which further contribute to the development of uterine fibroids.
Early Inception Of Menstruation:
When menstruation in women starts at a younger age, they have a longer lifetime exposure to estrogen. This extended period of exposure increases the likelihood of fibroid formation.
Diet And Nutritional Factors:
The diet of an individual plays a vital role in overall hormonal balance. Diets high in red meat and processed foods might increase the risk of fibroids. In contrast, diets rich in fruits, vegetables, and whole grains might have a protective effect.
Physical Inactivity:
An inactive lifestyle can assist in gaining weight and cause a hormonal imbalance. Regular physical activity assists in managing hormonal levels, improving blood circulation, and decreasing inflammation.
Stress and Hormonal Imbalance:
Long-term stress can also affect the balance of estrogen and progesterone hormones. These hormones might indirectly influence reproductive hormones, thereby contributing to the growth of fibroids.
Your Body Is Speaking – Are You Listening? Uterine Fibroid Symptoms Explained
Uterine fibroids are known for not causing symptoms sometimes, but whenever symptoms occur, they can differ based on the size, number, and location of the fibroids.
Menstrual Symptoms:
Women with uterine symptoms mostly face heavy uterine bleeding, which might need frequent changing of sanitary pads. Periods might also last longer than normal, leading to large blood clots being passed.
Pain and Pressure Symptoms:
Uterine fibroids can cause a feeling of heaviness or pressure in the lower part of the abdomen. Some women might face continuous pelvic pain or lower back pain.
Urinary and Bowel Symptoms:
Large uterine fibroids might press on the bladder, leading to regular urination or difficulty in emptying the bladder. Also, pressure on the rectum might also cause constipation.
Reproductive Symptoms:
Uterine fibroids can interfere with fertility and might increase the risk of miscarriage in some women.
Painful Intercourse:
Pain during sexual activity, also known as dyspareunia, is normally common in fibroids that are located near the cervix.
Back/Leg Pain:
Pain in the back or legs becomes more common if the uterine fibroid presses against the wall of the uterus.
Abdominal Enlargement:
Large uterine fibroids cause the abdomen to distend, sometimes making the individual look pregnant.
Large uterine fibroids might make the individual feel heavy and full all the time, especially in the lower belly.
Anemia:
Long-term heavy bleeding due to uterine fibroids can lead to iron-deficiency anemia, thereby making the individual tired, dizzy, and gasping for breath.
Uterine Fibroids Causing Symptoms?
Talk To A Specialist Now
Spotting The Invisible: The Path To Diagnosing Uterine Fibroids
The diagnostic process for uterine fibroids typically starts with physical evaluation of the patient, where the gynecologist might feel an enlarged or irregularly shaped uterus. Because uterine fibroids are asymptomatic, they are frequently discovered during regular check-ups.
If a gynecologist suspects uterine fibroids, they utilise various imaging evaluations to confirm the identification of the tumor, and ascertain the shape and size of the uterine fibroid.
Ultrasonography:
Is the most frequently utilized method for the identification of uterine fibroids. It makes use of sound waves to create images of the uterus and is completely safe and painless.
Ultrasound is mainly of two types, one is abdominal ultrasound performed over the abdomen. The other one is a transvaginal ultrasound that involves inserting a probe into the vagina to obtain clear images.
The ultrasound evaluation assists the gynecologist in ascertaining the size, number, and location of uterine fibroids and is mostly the first step in fibroid identification.
This imaging method provides in-depth pictures and is utilized in complex uterine fibroid cases.
This method allows gynecologists to look inside the uterus of the individual by utilizing a small camera.
Sonohysterography:
This method makes use of saline for better visualization of the uterus lining.
This method is very rarely used for the diagnosis of uterine fibroids, but it may be useful in certain situations, like incidental diagnosis, emergency evaluation, and detection of calcified fibroids.
Blood Tests:
These tests are mainly used to diagnose anemia caused by uterine fibroids, and also to rule out other bleeding disorders that might mimic uterine fibroids.
Hysteroscopy:
A thin, light scope is introduced through the cervix of the individual for better visualization of the uterine cavity. Hysteroscopy is considered to be the gold standard technique for examining the uterus.
Easing The Weight Within: Finding Relief From Uterine Fibroids
Treatment of uterine fibroids is based on how serious the symptoms of the disease are, the size of the fibroids, and the patient’s future pregnancy plans.
Treatment Through Medicines:
Treatment of uterine fibroids using medicines includes assistance in controlling symptoms of the condition. These might include pain relievers and hormonal therapies that decrease bleeding and cause the fibroids to shrink.
Uterine Artery Embolization:
Is a procedure to treat uterine fibroids that block the blood supply to fibroids, causing them to shrink and disappear.
Focused Ultrasound Surgery:
This method utilizes sound waves to damage fibroid tissue without the use of surgery.
Instead of using sound waves, this method makes use of heat energy to shrink and make uterine fibroids disappear.
Microwave Ablation is a minimally invasive therapy for uterine fibroids in which a thin probe is inserted into the fibroid, and microwave energy is used to generate heat and destroy the uterine fibroid
Hysteroscopic Treatment:
This removes fibroids through the vagina and cervix using a camera, with no external cuts, and is mainly used to treat fibroids inside the uterine cavity with a quick recovery.
Laparoscopic Treatment:
Uses small abdominal cuts to remove fibroids from the uterine wall, offering less pain and faster healing than open surgery.
Open surgery:
Involves a larger abdominal cut and is preferred for very large or multiple fibroids, but has a longer recovery period.
A surgical method in which only the fibroids are removed, and the uterus is preserved. This option is suitable for women who wish to have children in the future.
In this procedure, the entire uterus is removed through a cut in the abdomen. This method is considered when the uterine fibroids are very large, when symptoms are severe, or when other treatments have failed.
Total Abdominal Hysterectomy provides a permanent solution because uterine fibroids can never recur once the complete uterus is removed. However, this also means that women can never again become pregnant.
Choose The Right Treatment For Your Fibroids
Consult A Gynecologist Now
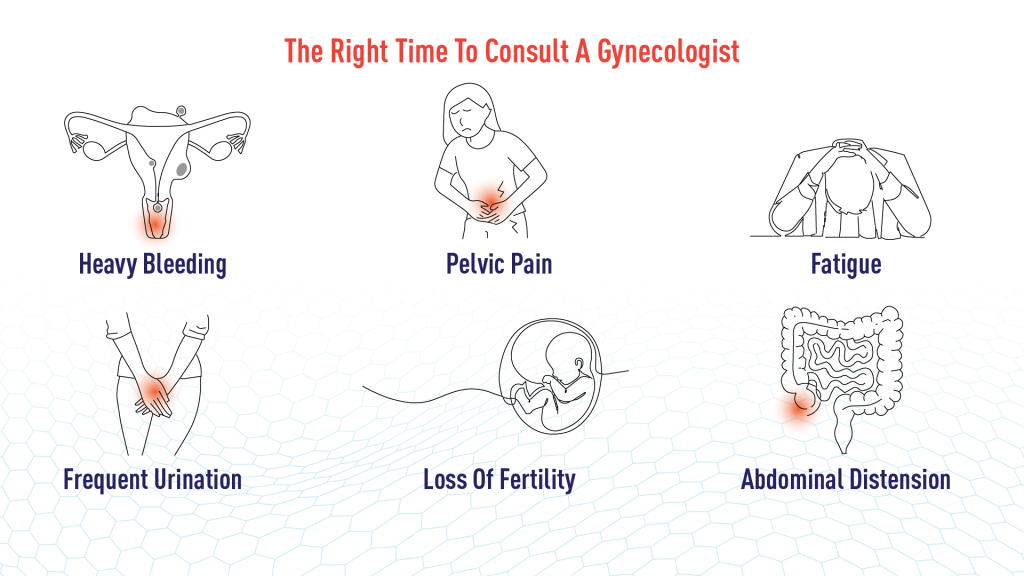
When Your Body Asks For Help: The Right Time For A Gynecologist
An individual should consider seeking the help of a gynecologist if she notices symptoms or changes that indicate a possible uterine fibroid issue.
Continuous Heavy Bleeding:
If the patient is experiencing unusually heavy menstrual bleeding or bleeding that lasts longer than usual and begins to affect their daily life.
Ongoing Pelvic Pain Or Discomfort:
If the patient feels constant heaviness, pressure, or pain in the lower abdomen that does not go away.
Frequent Urination Or Difficulty In Emptying The Bladder:
This happens when the uterine fibroids press on the bladder.
Unexplained Fatigue:
This can be a sign that the patient has become anemic due to long-term loss of blood.
Difficulty In Conceiving Or Repeated Pregnancy Loss:
Uterine fibroids can interfere with fertility and cause issues in a patient achieving pregnancy.
Noticeable Abdominal Enlargement:
The patient’s abdomen feels swollen or increases in size without a clear reason.
Symptoms after menopause:
If the patient has already undergone menopause and experiences any new symptoms like bleeding, pain, or discomfort, then they should get evaluated.
Little Daily Choices, Lasting Protection: Preventing Uterine Fibroids
While uterine fibroids cannot always be prevented completely, some lifestyle changes can assist in reducing the risk of their development or slow the growth. Making simple, continuous changes in daily life can help maintain hormonal balance and overall reproductive health.
- Individuals should maintain a healthy body weight through a balanced diet that includes fruits, vegetables, and whole grains, and limit red meat and processed food.
- Individuals should avoid a sedentary lifestyle and practice regular exercise for hormonal balance.
- Individuals should ensure that they take adequate vitamin D (Sunlight/Supplements if required).
- Individuals should manage and keep their blood pressure under check, because hypertension is one of the risk factors for uterine fibroids, especially in post menopausal women.
Individuals should practice relaxation techniques like yoga and meditation to keep stress under check. - Individual should schedule and attend regular gynecological check-ups, and stay aware of changes in their body and act quickly.
Take Early Action Against Fibroids
Reach Out To A Specialist
The Strength You Carry Should Be Greater Than The Adversity You Face:
Dealing with uterine fibroids can sometimes make you feel that you are being overpowered, especially when signs of the fibroids affect your daily peace of mind. Nevertheless, it is vital to remember that uterine fibroids are a common and manageable condition. With the right knowledge, timely identification, and precise treatment, most women regain control over their health and thereby lead a comfortable life.
Every Challenge That Your Body Faces Is A Chance To Care For It In A Better Way
















 Appointment
Appointment Call
Call More
More