Ileostomy in a premature twin girl born with low birth weight

This is the story of a little fighter we got to witness in our unit. Babies like this strengthen our faith in clinical medicine and outcomes.
The child was born to a 28-year-old-first-time-mother. The mother conceived twins naturally and went into labor pains about 2 and a half months prior to expected dates. She was delivered in a nearby maternity nursing home. Their birth weights were 1kg and 800g. The premature delivery was caused due to maternal urinary tract infection. This particular scenario strengthens the observed advances in perinatal care in the form of antenatal steroids and maternal cervical swab surveillance. Antenatal steroids make the babies more mature and cervical swab gave us a headstart on what infection baby is likely to harbor in the first 3 days of life.
The babies were retrieved from the nearby hospital at a half hour of life. This was the first neonatal transport at Yashoda Mother & Child Institute. Babies were covered in warmth providing embrace bags and were transported with PEEP support (Positive end-expiratory pressure). PEEP is needed for the stabilization of alveoli and lack of it causes increased work of breathing, worsening distress, and destruction of surfactant.
The baby for today’s discussion is the smaller of the twins, who weighed only 800g. She was stabilized on minimal CPAP and did not require mechanical ventilation or surfactant therapy on day 1 of life. Attempts were made to start on minimal feeds on day 2, however since the baby did not tolerate feeds, baby continued Nil-by-Mouth (NPO, nil by ps). This minimal feed intolerance is common among preterm babies. Central lines were secured on day 3 and x-ray done, which revealed a small air pocket under the diaphragm. With a lag period of just 45 minutes, the baby was shifted to OT. This included the confirmatory x-ray, mobilization of pediatric surgeon and anesthesia team.
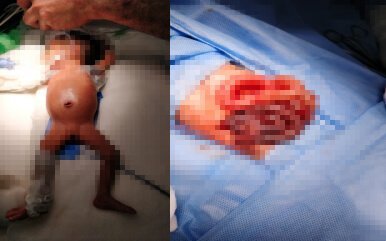
Ileostomy
On the OT table, the baby was accompanied by the neonatal team and was found to have multi-segment perforations. This is very unusual for neonate on day 3-4 of life. This is a usual presentation on day 7-21 of life but not in the first week of life. The most probable cause of this presentation was a community-acquired E.Coli infection in the form of urinary tract infection, which would have spread to the baby, not only causing the prematurity but also almost deadly multiple perforations.
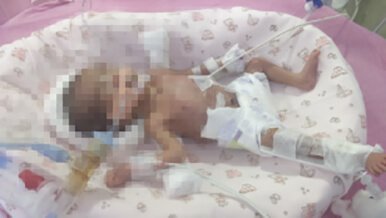
Ileostomy in neonate
This leaves us to introspect about the rampant use of antibiotics and the resulting spread of multidrug-resistant bugs even in the community. This particular E.Coli was resistant to most of the drugs suitable for use in neonates, leaving us with choice of Meropenam and Colistin.
The baby was stabilized post laparotomy, resection, and ileostomy. She was managed under NPO status for 14 days and then was started strictly with breast milk alone. This is the youngest and smallest baby who went under the knife in Yashoda Mother & Child Institute. The baby was in the neonatal ICU for 56 days and discharged at almost double the birth weight.
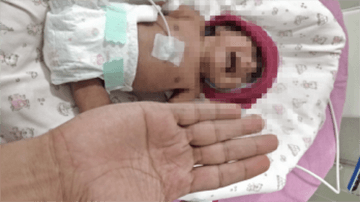
Premature low-birth baby
The baby was put under careful close monitoring during the post-discharge period. At 5 months of life, the baby presented with increased outputs from the stoma and loss of essential minerals. The child also had viral Lower Respiratory Tract Infection (LRTI). During the hospitalization, the stoma also began to prolapse. With the complications of stoma losses and the prolapse of the stoma, the baby was operated to close the stoma with a weight of 1.68 kg at admission. The baby was treated for LRTI, stoma was closed and the baby is currently 2 kg.
This little baby has taught us so many things about medicine, ethics, the justification for care and belief in the outcomes.
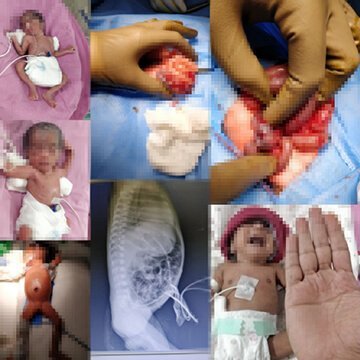
Ileostomy in premature baby
About Author –
Dr. Balla Kalyan Chakravarthy, Consultant Neonatologist Pediatrician, Yashoda Hospital, Hyderabad.
MD (Pediatrics), DM (Neonatology), Fellowship in Perinatology
His special interest lies in neuroprotective strategies, child nutrition, infection control & non-invasive ventilation. His services include pediatrics, neonatology & NICU services and perinatology/high-risk obstetrics counseling.






 Appointment
Appointment Call
Call More
More