Yashoda Hospitals > Diseases & Treatments > Gynecology & Obstetrics > Polycystic Ovary Syndrome – PCOS or PCOD
Polycystic Ovary Syndrome – PCOS or PCOD
Its causes, symptoms, diagnosis and treatment
Things you need to know about PCOS or PCOD
What is PCOD (Polycystic Ovarian Disease) / PCOS (Polycystic Ovary Syndrome)?
Polycystic ovarian syndrome or disease (PCOS/PCOD) is a hormonal disorder that affects women in their reproductive age. PCOS is a common health condition that affects teen and young women, it is sen in 1 out of o10 women in their childbearing age. The reproductive system of women is controlled by the complex interplay of primarily five reproductive hormones namely estrogen, gonadotropin-releasing hormone, follicle stimulating hormone, progesterone and luteinizing hormone. An imbalance within these hormones leads to a hormonal disorder called the polycystic ovary syndrome (PCOS) or polycystic ovarian disease (PCOD) among women of reproductive age.
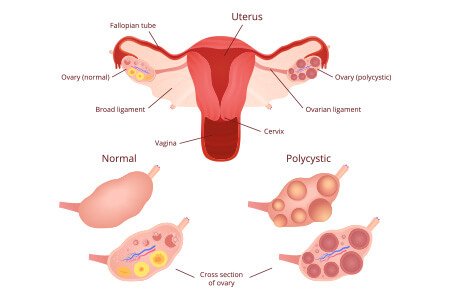
Polycystic ovarian syndrome is marked by the breakdown of reproductive hormones in women of childbearing age. Along with havoc in female hormonal control, ovaries release abnormal amounts of androgen (male hormones). This hormonal breakdown results in irregular or prolonged menstrual periods, excessive body hair, acne and hair loss. Polycystic ovaries may fail to develop follicles and regularly release eggs, causing difficulty in conceiving a pregnancy.



 Appointment
Appointment Call
Call More
More